On the day he was scheduled for a COVID-19 vaccination, 77-year-old Jaikishan Ram wrapped himself in a well-worn wool jacket, cap, and sweater to prepare for the three-hour trek down the mountain.
To access the main road from his home high in the Himalayan mountains of the Indian state of Uttarakhand, Ram had to first climb down a mile of steep, unpaved, sloping path. From there, it was another 90 minutes on the main road to the village of Padampuri. That’s where the only government hospital and walk-in COVID-19 vaccination center in the Dhari area—home to some 30,000 people spread across 46 villages—is located.
It was early September, and India was still recovering from a devastating second COVID-19 wave, driven primarily by the Delta variant. According to official government figures, more than 400,000 Indians died between June 1, 2020, and July 1, 2021, but a recent report in the journal Science estimated that the true toll might have been as high as 3.2 million deaths. The majority of those—2.7 million—occurred in three months, April through June 2021.

In the following months, cases of COVID-19 dropped significantly, and hospitalizations remained relatively low even during an Omicron-driven third wave, which peaked in late January. This is in part thanks to nationwide efforts to stop the virus. India began rolling out COVID-19 vaccines in January 2021, starting with health workers, then for people over 50 and those with comorbidities. It took a while for the vaccine rollout to pick up pace, but by Jan. 30 of this year, India’s government said 75% of its adult population had received two doses of a COVID-19 vaccine.
Read More: How Did India’s COVID-19 Crisis Become a Catastrophe?
As a septuagenarian, Ram was eligible early on, but at first he stayed home. He’d been unwell and felt uncertain about the safety of the vaccines. He was also wary of the trip he’d have to take to get his shots. But months of persistence by the health workers in Padampuri—and especially by his daughter-in-law, who is part of Dhari’s vaccination team—managed to persuade him. “I saw how hard she worked on this,” Ram says. “She urged me to take the vaccine, if not for myself, then for my family and the community.”
His change of heart wasn’t unusual. Despite early concerns, in this isolated region that spans more than 30 sq. mi.—most of it rugged terrain that rises to 7,000 ft. of elevation—by the beginning of October, 100% of eligible adults had received a first dose of a COVID-19 vaccine. That equates to some 28,000 people, according to Himanshu Kandpal, the chief medical officer of the Dhari area, who is in charge of Padampuri’s medical center. The state of Uttarakhand as a whole reached that same milestone in mid-October, with all eligible adults—some 7.4 million people—receiving a first dose, usually of the Oxford-AstraZeneca vaccine, known locally as Covishield. (Those vaccinated in the very first phase typically received Covaxin, India’s own vaccine.)
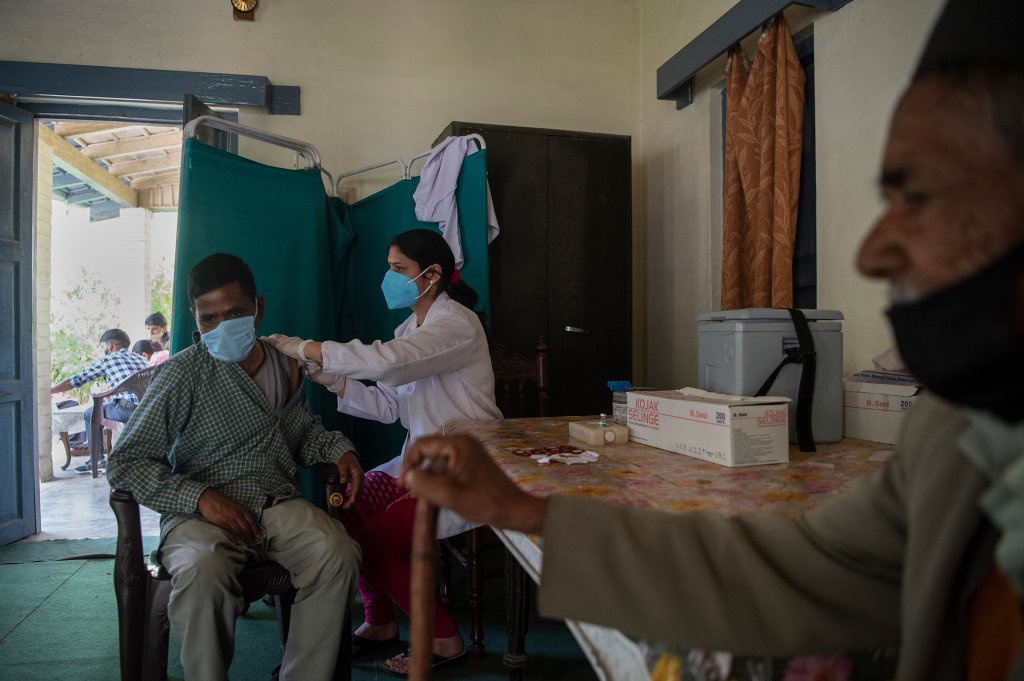

While most Indian cities are now catching up, Dhari was an early success story, and continues to get people to show up—more recently, for their second doses and booster shots. As of the time of writing, over 80% of eligible adults in Dhari, one of the most remote places in the world, have received a second dose, despite heavy snowfall and road closures in hilly areas. Kandpal says that by the end of February, the adult population in the region will be fully vaccinated—though it’s difficult to be completely certain in a region where officials struggle to document the members of every household. All eligible teenagers of ages 15 to 17 have also received a first dose.
Other districts in the state have had similar success, as has India’s northernmost mountainous state of Himachal Pradesh. Indeed, the vaccination rate in Dhari and other hill districts far outstrips those of much richer places with better health infrastructure and where vaccines are widely and easily available. In the U.S., for example, 64.4% of adults have been fully vaccinated as of Feb. 14, while 75.9% have had a first dose.
How did a remote Himalayan region manage to succeed where so many other cities and countries have struggled? The answer underscores the value of health workers who are embedded in their communities and know how best to serve them in a crisis.

At first glance, Dhari seems an unlikely place to hit such a vaccine-success milestone. For one thing, the Indian government made a smartphone app the primary means for booking a vaccination appointment—in a country where only around half of the population has a smartphone. In rural areas like Dhari, that proportion is far lower.
Another challenge was simple practicality. “Much of the population here lives in remote areas, and it takes them so long to come to the medical center,” Kandpal told TIME in August, sitting in his office in Padampuri—the only significant medical facility for 25 miles. The building, covered in faded yellow paint, stands atop a mountain slope, approachable only by a long flight of steep stairs carved out of the mountainside. At about 5,200 ft. of elevation, it is thousands of feet below many of the mountain villages it serves. “People have to commit to a full day to get vaccinated. That didn’t help,” Kandpal said.
Hema Devi knows just how difficult that can be. In July, the 45-year-old farmer made the steep mile-long uphill trek from her home in the remote hamlet of Thiroli, to a vaccination camp in the bigger village of Dhanachuli. She waited for hours for her turn, before learning that the camp had just run out of vaccines. “I hear about people not taking the vaccines in the cities, and I am puzzled,” she says. “They don’t even have to climb a mountain or negotiate broken roads. They also don’t have to think of who’s going to cook dinner or lunch if they are stuck at the camp—they can just order food on the phone.”


On Aug. 2, she tried again, waking before dawn to cook, clean, and take her buffaloes and goats out to graze before setting off with her husband and two neighbors. When they arrived in Dhanachuli, Devi and her husband joined different lines to register for their shots. The line for men was much shorter, with most of them—including Devi’s husband—there to receive second doses, while most of the women had yet to receive their first.
That disparity has persisted across India, in part because of the difficulty in getting time away from housework and childcare. According to India’s official vaccination website CoWIN, as of Feb. 14, a total of 1.67 billion vaccine doses have been administered in India: 49.5% to women and 50.5% to men—a gap of some 38 million doses.
Indeed, when Devi’s husband received his first dose in July at the primary health care center in Padampuri around an hour’s drive away, she couldn’t go with him because of home responsibilities. “It would have taken the whole day, and who would have taken care of the children and the housework?” Even on the day Devi finally received her vaccine, she rushed home after registering at the camp, to cook lunch and tend to the livestock while her husband saved her spot. She sprinted back just in time for her shot. “I didn’t want to miss out this time too,” she says. “If we run out of vaccines, you never know when we will get it next.”

Devi wasn’t always so eager to get the vaccine. Like many Dhari residents interviewed by TIME, she was initially scared. “We heard stories of infertility and deaths,” she says. “But then we saw people taking it and they were OK. Also the health workers came to the village and explained and encouraged us. They are one of us, so we trust them.”
Crucially, these workers have history on their side. The health care workers in Dhari are mostly local women who have been trained to act as educators in their communities through work as accredited social health activists (ASHAs) or hired by the government as nurse-midwives (ANMs) to act as the first point of contact between the community and the public health care system. Across India, especially in rural areas, these community workers have played a crucial role in the pandemic, creating awareness about the virus, tracking and monitoring cases, and then rolling out the vaccination program. In Dhari, this well-earned trust led locals to buy into the idea that they needed to get vaccinated to protect themselves and their families against COVID-19—even if it meant trekking hours through steep terrain.
The success of Dhari’s COVID-19 vaccination campaign was also built on years of outreach within remote communities, especially among women and children, notably through India’s robust universal immunization program that reaches around 26.7 million newborns and 29 million pregnant women each year. That program relies on a broad network of district hospitals, primary health centers, government health workers, and community volunteers. It’s also credited with the country’s incredibly successful polio-vaccination campaign, which began in 1994, when India accounted for around 60% of global polio cases. Millions of frontline workers took on the task of vaccinating 170 million children under 5, twice a year. In 2014, two decades after the campaign began, India was declared polio-free.


India’s immunization program for children may be “a well-oiled machine,” says Rajib Dasgupta, who heads the community health program at Jawaharlal Nehru University, but the system still needed to be adapted to deploy COVID-19 vaccines to adults. Kandpal and his team of 13 ANMs and 46 ASHAs consulted with village heads across Dhari to tweak the existing immunizing infrastructure to address the practical issues around travel and the lack of smartphones. First—and long before most areas in India began doing so—they decided to send out mobile teams to villages because not enough people were coming down to the two walk-in centers. While the polio-vaccine program includes a follow-up door-to-door campaign, this was a significant scaling-up to cover the entire adult population. These new mobile teams were capable of trekking into the mountains to get closer to isolated communities, where they established pop-up vaccination sites designed to get more shots into arms—both for those people who already want it and those who aren’t so sure.
Read More: How the Pandemic Is Reshaping India
Kandpal’s team also added fully equipped ambulances to the mobile teams in case of adverse reactions to the vaccines, a data-entry operator to register the villagers on the government vaccine app, and a pharmacist to hand out acetaminophen and advise people on what to expect after their shots. Kandpal also set up a WhatsApp group between local health workers and the village heads, posting the weekly vaccination schedule so that village heads could communicate with villagers. “COVID taught us to think out of the box. The systems it forced us to create will go a long way in the future too, to cater to this population,” Kandpal says. “We have taken an existing but old resource and modernized it.”
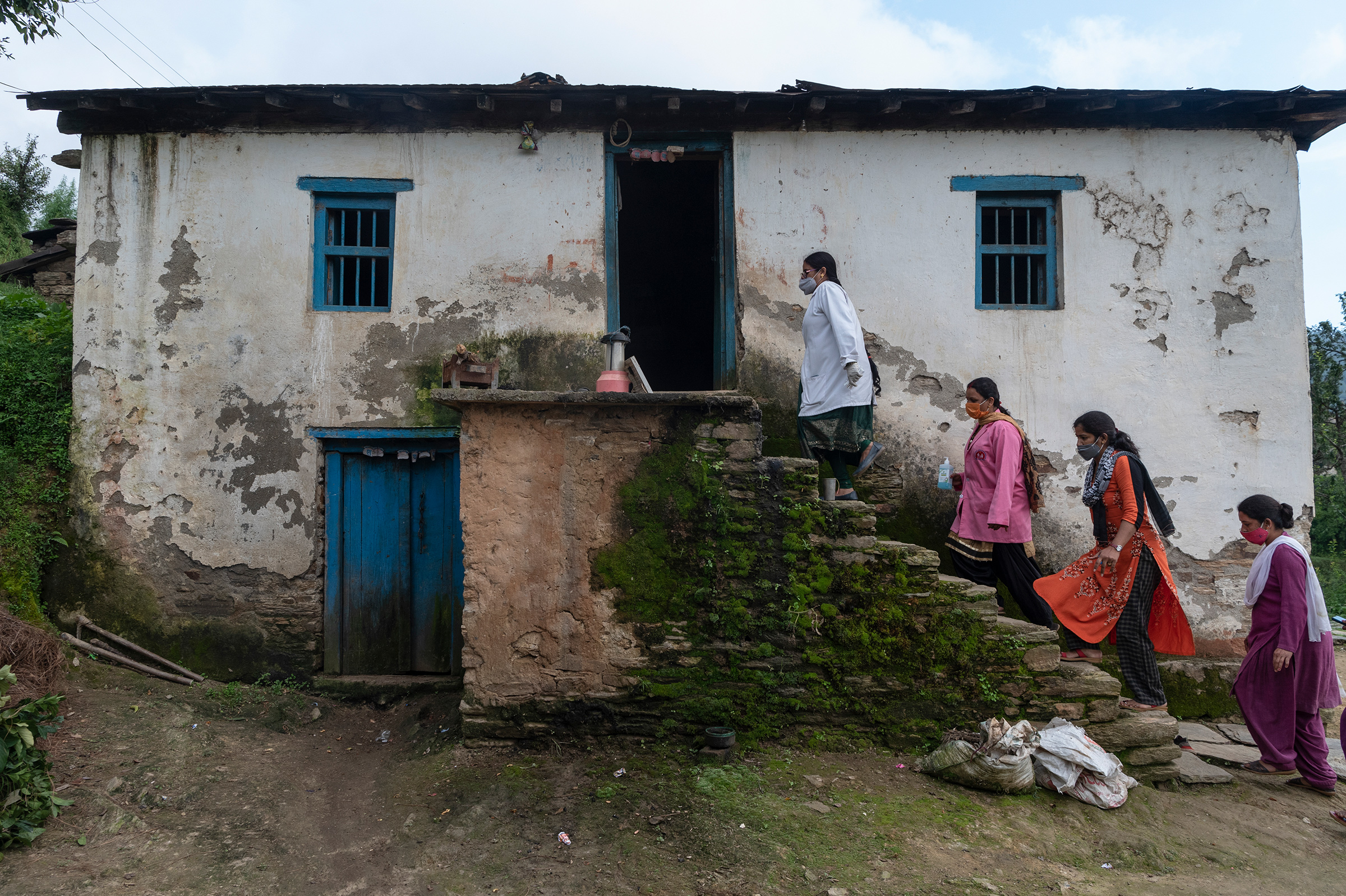
On Sept. 4, nurse-midwife Renu Sharma—a member of Kandpal’s team who has been working with the Dhari population for 13 years now—traveled with a team of health care workers from Padampuri to the remote village of Aghariya. There, she received a warm welcome. She knew lots of the women by name, having vaccinated their children years earlier, and in a mock-stern voice, she told them to come and get their own COVID-19 vaccines at the camp now.
Before the arrival of Sharma and her team, the nearest place for Aghariya residents to get vaccinated was the camp in Dhanachuli—a tough journey along an unpaved path that could be particularly treacherous whenever rains loosened the rocks and soil. That’s why Sharma and her team decided to set up a temporary pop-up vaccination site in Aghariya. They were quickly inundated, and by the afternoon the line for vaccines continued to grow.
While administering shots, Sharma noticed a group of three elderly men who had spent the day sitting at the pop-up vaccination clinic. During a lull in activity, she approached them. “Bubbo, have you registered?” she asked, using a local term of respect meaning grandfather. They demurred. “No, no, we came here just to see what’s happening,” one said. “We don’t want to take the vaccine.”
Undeterred, Sharma continued to press: “Look at me, bubbo, I was one of the first ones to take the vaccine. Has anything happened to me?” she said. At that point, others in the village who had gotten a shot joined in, saying they too had suffered no serious side effects. Finally, the men relented. Sharma marched them to the registration table with a triumphant smile and went back to her station to open up another pack of the vaccines. “Sometimes you have to persist with them a bit,” she said. “I have had to persist for days and weeks with some people.”

At the end of the day, Sharma consulted her list of village residents and checked them against those who had registered to be vaccinated. She found the names of three elderly and disabled people with mobility issues who she knew couldn’t make it to the camp. She took a bag with vaccine doses and supplies and walked with her team toward their homes, a short trek from the vaccination site. An official door-to-door vaccination policy would only be announced by Prime Minister Narendra Modi in another two months, but Sharma’s prior work had taught her that sometimes you need to meet people where they are.
Health workers like Sharma know well the challenges in the smaller communities they serve, whether travel difficulties or household commitments—a kind of knowledge and intimacy that is impossible in bigger cities. At the Aghariya camp, she did not waste an opportunity to advise mothers who were there for routine immunizations for their kids that they should also get the COVID-19 vaccine for themselves. “You have to be mindful of the community’s sentiments,” she says. “We don’t push too hard. It takes time. Sometimes I request, sometimes I am stern. But they know I mean well.”
Throughout the last months of 2021, Sharma and others like her worked unremittingly to get vaccines to people in remote villages. Hema Devi, who got her first shot in August, was able to get her second in December—though she still had to make the long trek from Thiroli to Dhanachuli. She was relieved to get it when she did, as an Omicron-fueled surge of COVID-19 cases began sweeping the country shortly after.
Several weeks later, India’s COVID-19 cases are on the decline, and state governments are reopening schools after long hiatuses. In Dhari, where cases are also falling and hospitalizations remain relatively low, health workers are still working to fully vaccinate 15- to 17-year-olds, as well as administer booster shots to adults. Though cases are now falling and hospitalizations have remained relatively low, health workers in Dhari are still working to fully vaccinate 15- to 17-year-olds, as well as administer booster shots to adults. Sharma says it’s much easier this time than with first doses because there’s a much greater understanding of the need for them. Villagers have “watched the news about the booster dose on television and have been coming up to me asking about it,” she says. “They understand the importance of the vaccines in keeping the whole community safe.”
That understanding helps people like Devi to walk the extra mile to get vaccinated. “If I could, I would urge everyone to take the vaccine. Don’t think of yourself; think of your friends and family and your community,” she says. “If you are safe, they are safe; the world is safe.”
—With reporting by Eloise Barry/London
More Must-Reads From TIME
- What Student Photojournalists Saw at the Campus Protests
- How Far Trump Would Go
- Why Maternity Care Is Underpaid
- Saving Seconds Is Better Than Hours
- Welcome to the Golden Age of Ryan Gosling
- Scientists Are Finding Out Just How Toxic Your Stuff Is
- The 100 Most Influential People of 2024
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Contact us at letters@time.com
