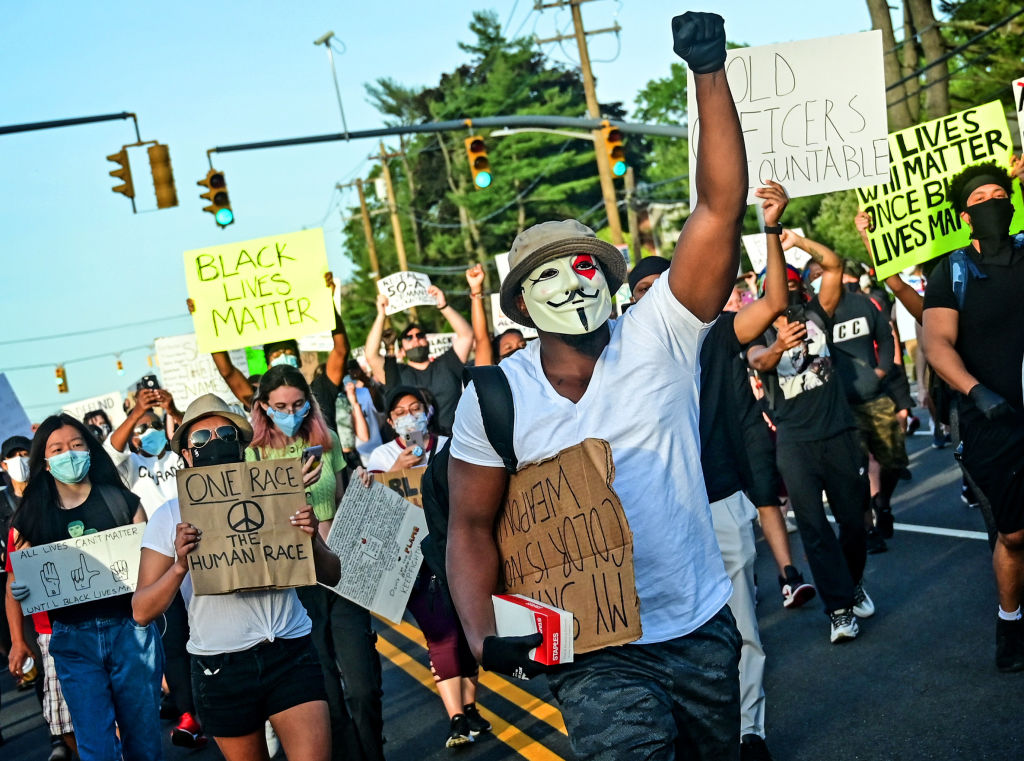
State and local public health officials are in a tough spot. After months of imposing restrictions to protect their residents from the highly infectious coronavirus—at great cost to families’ livelihoods and the broader economy—they now must balance those efforts with another, equally vital imperative: protecting Americans’ right to gather en masse to protest police brutality and systemic racism.
This balancing act is further complicated by timing. New daily cases of COVID-19 worldwide hit a record high on June 7, according to the World Health Organization, indicating that the pandemic is perhaps worsening. And after months of stay-at-home orders to slow the spread of the disease, many states and counties are just now beginning to reopen their economies, despite ample evidence many of them have not yet met containment benchmarks, further increasing the likelihood of an uptick in new infections nationwide.
In response to this confluence of factors, public health officials are performing something of a high-wire act. In most states and regions, political leaders have refused to discourage the protests, and are instead moving to prepare local hospitals, testing sites and contact tracing forces for what many predict will be a resurgence of COVID-19 across the country. But just as the danger of the virus itself has not changed, neither have the funding or organizational obstacles that left states scrambling in the early months of the pandemic.
Now, as two crises that disproportionately impact black Americans collide—one, the pandemic, and the other ongoing police brutality—officials predict that the country’s patchwork response could mean a rocky, and perhaps deadly, road ahead.
Weighing the risk
In the days and weeks after George Floyd’s killing by Minneapolis police sparked mass protests, most governors, mayors, physicians, epidemiologists and local health commissioners did not condemn the gatherings or encourage participants to go home. Instead, mayors from Atlanta to Oklahoma City to Washington D.C. joined marchers, while city employees in Minneapolis, New York, St. Louis and Baltimore distributed masks to demonstrators. Nearly 1,300 public health workers signed an open letter calling the protests “vital to the national public health and to the threatened health specifically of Black people in the United States.”
But these acts of solidarity were not taken lightly, public health experts tell TIME. While the threat of COVID-19 has not diminished, the circumstances have shifted, requiring protesters, and thus officials, to make informed calculations about the relative threats to public health and safety. “The impact of systemic racism over centuries is far greater than the impact of COVID,” says Julia Marcus, an infectious disease epidemiologist at Harvard Medical School. “And if we can make progress toward dismantling structural racism in a moment of collective action, then that actually could have a positive impact on public health.”
But, Marcus adds, state and local officials must also work to encourage protesters to gather as safely as possible. “What we should be doing right now is very clearly communicating the risks and ways that people can reduce any potential harms,” she says. For example, on June 6, the New York City Department of Health and Mental Hygiene released recommendations for protesters, encouraging people to use noisemakers instead of singing or chanting, carry hand sanitizer, and avoid contact with vulnerable people after attending demonstrations. Public leaders in many cities have encouraged residents to get tested for COVID-19 after they participate in protests.
Police interactions
While many protesters nationwide appear to be wearing masks, not everyone is doing so. And police officers’ actions can make things worse, public health experts say. Photos and videos across the country have shown police officers not wearing masks, and other police actions, like corralling demonstrators, spraying chemical irritants that produce tears and coughing, and crowding people into vans and jails can exacerbate the spread of the virus. In Chicago, Rossana Rodriguez-Sanchez, an alderman for the city’s 33rd ward, spent hours at a precinct helping release on bail detained protesters last week and told TIME “there was not a single officer wearing a mask.”
Taylor Barros, a 16-year-old who was arrested at a protest in Brooklyn, told TIME that the police officers she interacted with acted inconsistently regarding mask usage. “As soon as we got on the bus, they removed my bandana from my face because the cops said I could choke myself,” Barros said. Another officer later handed out masks to those in custody.
Department protocols require New York City and Chicago police officers to wear masks during the pandemic. The NYPD previously told TIME it was “working as fast and safely as we can to process arrests during this unprecedented time.” A spokesperson for the Chicago Police Department told TIME that in addition to requiring masks and gloves outside, it is “strongly recommended” that officers wear these items inside precincts and department vehicles, but acknowledged that given “the heightened activity that officers have been responding to in the past week,” those recommendations have not always been followed.
Keep up to date with our daily coronavirus newsletter by clicking here.
Preparing for a surge
Research shows it can take up to 14 days for those newly infected with the coronavirus to exhibit symptoms of the disease. As a result, epidemiologists expect that cases linked to the ongoing protests will begin appearing in the next week or two. But, they warn, the data is muddy: already, almost half of states are seeing an uptick in coronavirus infection rates, likely tied to the lifting of stay-at-home orders beginning in late April and May. By June 9, at least 22 states had increasing COVID-19 cases.
This dynamic—a bump in infections due to reopening, combined with another expected rise due to protests—means that states are again scrambling to prepare for an increase in hospitalizations. But in early June, some cities and regions are much better prepared than others. NYC Health + Hospitals, the corporation that operates New York City’s public hospitals, said that if the city, the epicenter of the outbreak, sees another spike, it is “prepared to re-activate strategies it implemented in late-March/early-April to respond to COVID-19.” These steps included nearly tripling ICU capacity, reassigning doctors to treat coronavirus patients and recruiting additional clinical support, a spokesperson said.
In Minneapolis, doctors say they are also on track to handle a surge of new cases. Abbott Northwestern Hospital, which is near where Floyd was killed, has not taken specific steps in response to the protests, but Dr. Timothy Sielaff, chief medical officer of Allina Health, which runs the hospital, said the health system is ready to scale up its response if needed. “Allina Health has been actively preparing for a surge in COVID-19 patients for the last few months,” he said in a statement. “We have solid plans in place and will run the plans in accordance with patient volumes.”
Data suggests that other parts of the country where cases are increasing are less prepared. Thirty two states had low ICU availability on Tuesday, according to data from Covid Exit Strategy. Hospitals in Montgomery, Alabama have gotten so crowded they had to send patients to other parts of the state, and metropolitan areas such as Phoenix and Memphis are projected to run out of ICU beds in three weeks, according to the COVID-19 Burden Index, run by the health care intelligence firm Leavitt Partners.
In Arizona, the state health director urged hospitals on June 6 to “fully activate” their emergency plans and to reduce or suspend elective surgeries. That directive came one day after Banner Health, the state’s largest health system, told reporters its ICUs are “very busy” and that if trends continue, the system would soon need to exercise its surge plan. By June 8, Banner Health said it also recently reached capacity on extracorporeal membrane oxygenation (ECMO) machines, which act as external lungs for patients with severe lung damage, a potential complication of COVID-19.
Racial disparities
As local governments make their preparations, public health officials say hospital care, testing and contact-tracing efforts must be designed carefully to reach out to Black Americans, who have been dying at a much higher rate from COVID-19 than white people, and who express lower rates of trust in public institutions. “Black and brown people are especially aware of the unethical treatment that happens, and the ways in which even public health policies have been complicit in exacerbating health disparities,” says Lorraine Dean, an assistant professor of epidemiology at Johns Hopkins University who studies racial health disparities.
Dean notes that actions by the federal government—from President Trump’s defense of white nationalists in Charlottesville to his administration’s slow response to the current pandemic—make it harder for people to trust their local governments and health departments too. “If there’s already a distrust of the U.S. as a whole, and U.S. systems as a whole, the health care system is a part of that,” she says.
Some states have taken proactive steps to address this trust gap. The Minnesota Department of Health, for instance, is working to set up voluntary COVID-19 testing sites for anyone who participated in mass gatherings such as demonstrations, clean-ups and vigils, and New York Gov. Andrew Cuomo said on June 7 that his state was adding 15 testing sites for protesters and that New York City would conduct 35,000 tests a day so that demonstrators can better protect themselves and their families. Atlanta added free testing sites for protesters on June 6. Public health officials in other large cities have frequently reminded residents they can now get tested for COVID-19 even without symptoms.
Even before the protests, Baltimore started piloting three mobile testing sites that do not need appointments or doctor referrals, in addition to its other community testing sites. The city used print fliers and radio ads to reach parts of the community who may not be on social media, and these continue to be options for people who want to get tested after attending protests.
A trust gap
The next step is contact tracing, which entails workers identifying anyone who has come into contact with an infected person, and then providing guidance on quarantining, medical treatment and other services. This tracking is widely considered indispensable to slowing the spread of COVID-19. U.S. Centers for Disease Control and Prevention Director Robert Redfield told Congress on June 4 that in order to control the next wave of COVID-19, the U.S. needs an army of between 30,000 and 100,000 contact tracers. While many cities have begun hiring rafts of new contract tracers, they’re still largely playing catch up.
A few weeks ago, Los Angeles had just 400 of the 6,000 contact tracers it estimated it would need for California’s reopening, while New York City launched its contact tracing program on June 1 with 1,700 workers after Mayor Bill de Blasio said in early May he aimed to have 2,500 by early June and eventually hire between 5,000 and 10,000 contact tracers. Philadelphia’s Department of Public Health, which created a new contact tracing division, currently has only about a dozen contact tracers on staff, the department told TIME. In Columbus, Ohio, health department staffers have been reassigned as contact tracers and have seen their workloads increase significantly in recent weeks. John Henry Jr., an HIV counselor currently doing contact tracing there, told reporters at a press briefing on June 4 that a few weeks ago, he was supposed to reach about a dozen contacts each day, and now he has to call as many as 30 contacts daily.
As police continue to arrest—and in some cases abuse—protesters, public health officials say contract tracers face an uphill battle. Protesters, many of whom are already distrustful of police and public authorities, may be unwilling to provide government workers with the names and contact information of friends or colleagues with whom they were protesting. “I fear that there will be even less uptake, especially in communities that really do need the most contact tracing,” says Dean, the expert at Johns Hopkins. “I definitely think that distrust of the health care system that already existed and was warranted—there’s no reason why it shouldn’t continue to play out when it comes to COVID.”
Baltimore Health Commissioner Dr. Letitia Dzirasa told TIME that her city is working to bridge the trust gap. “Even leading up to this point, we tried to be somewhat intentional about our messaging around contact tracing and tried to indicate that we’d never ask for certain personal information, like social security or credit card number or immigration status,” Dzirasa says.
On June 4, Baltimore announced it would hire some 300 additional contact tracers to support the roughly 100 full-time and 28 part-time staffers it had already put on the task. The city is also partnering with trusted local figures such as church leaders, community organizers and peer recovery specialists to help tell residents about the importance of everything from mask-wearing to contact tracing. This last part is perhaps the most essential: “We recognize that we may not get the accurate answer every single time,” Dzirasa says. “But I think it’s important that we continue to make the effort and build trust within the community and say, ‘Please let us know who you’ve been in contact with.’”
Effective contract tracing, after all, may be one of the only ways to encourage mass public protests while also containing the rampant spread of a deadly disease.
— With reporting by Andrew R. Chow/New York
Please send any tips, leads, and stories to virus@time.com
More Must-Reads from TIME
- Introducing the 2024 TIME100 Next
- The Reinvention of J.D. Vance
- How to Survive Election Season Without Losing Your Mind
- Welcome to the Golden Age of Scams
- Did the Pandemic Break Our Brains?
- The Many Lives of Jack Antonoff
- 33 True Crime Documentaries That Shaped the Genre
- Why Gut Health Issues Are More Common in Women
Write to Abigail Abrams at abigail.abrams@time.com