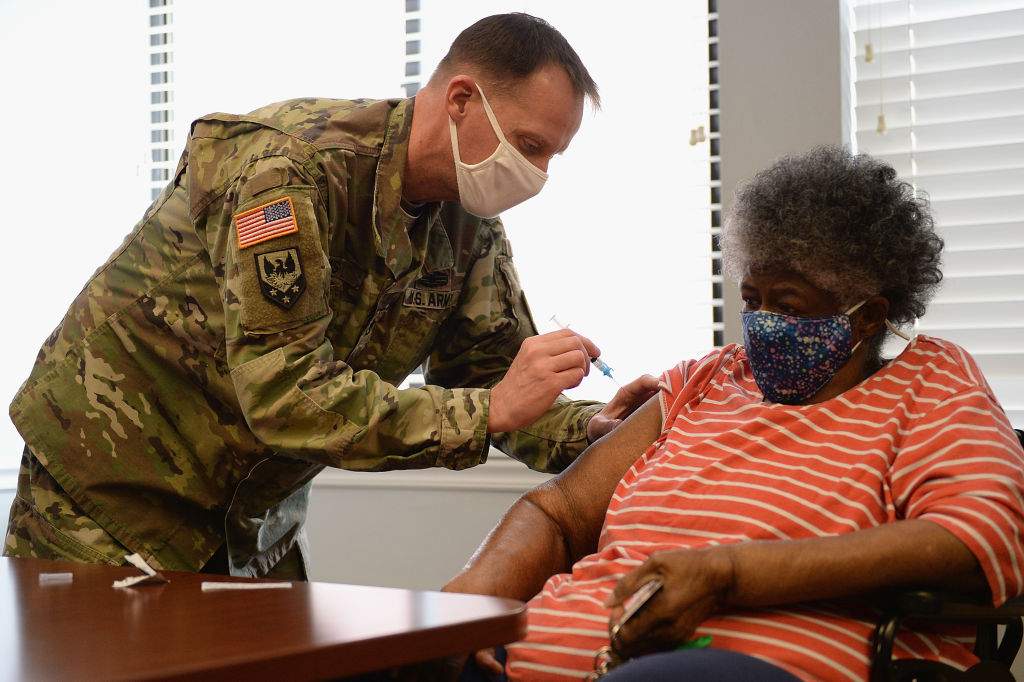
In mid-June, U.S. maps tracking the spread of COVID-19 began showing a cluster of cases growing in the middle of the country. The epicenter lay in Missouri, particularly its more rural and remote areas. At the time, Missouri had something that other states didn’t: the Delta variant.
To be fair, the highly transmissible Delta variant had at that point already crept into other states. But it had truly established itself in Missouri. Among the 25 states the U.S. Centers for Disease Control and Prevention (CDC)’s website reported on at the time, Delta was showing up in less than 5% of swab samples in 15 of them. Colorado had the second-highest rate, at 12%. But Missouri was something else: nearly 30% of COVID-positive swabs were linked to the Delta variant. As of July 28, Missouri is reporting a seven-day average of new daily cases of 27.3 per 100,000 people, up from 5.4 during the first week of May, before Delta took hold there.
In the weeks since, the Delta variant has become, or is on the brink of becoming, the dominant variant in every region of the continental U.S. The CDC is now reporting that Delta is so prevalent in the region encompassing Missouri, Iowa, Kansas and Nebraska that it’s now effectively the only variant, accounting for an estimated 96% cases. These states, and others with high levels of Delta, including Florida, Louisiana and others in the Gulf region, are now seeing overall cases spike.
As the first U.S. state to suffer a major Delta outbreak, Missouri is a harbinger for other regions of the country that also have low vaccination rates and a mix of rural areas and small towns with a handful of mid-sized cities—which is to say, much of the country. The following charts demonstrate the strength and swiftness of the Delta strain in a state particularly vulnerable to an outbreak—and why our efforts to stay ahead of the virus aren’t working.
Where Delta took hold
Missouri has a relatively low vaccination rate, with 41% of the population fully dosed as of July 26, compared to about 50% nationwide and 67.3% in Vermont, the most-vaccinated state. But Missouri’s vaccinated population isn’t uniformly distributed across the state. Boone County, home to 180,000 people and the state’s largest university, has the highest vaccination rate among Missouri counties at 48%. Places with larger populations like Kansas City (39%), St. Charles County (45%) and St. Louis County (also 45%) help pull the overall state vaccination rate higher.
But in smaller and generally more rural counties—that is to say, most of the state’s geographic area—vaccination rates drop off, leaving residents vulnerable. The below chart, which includes counties and cities with more than 20,000 people (collectively accounting for nine in 10 Missourians), shows that places with the highest COVID-19 case rates tend to be smaller counties with lower vaccination rates.
What this chart doesn’t show is how much the Delta variant is to blame for Missouri’s high overall case rates. That’s because not all positive COVID-19 test swabs get sent to the lab for genomic sequencing—health agencies use only a random sample of swabs to estimate a variant’s prevalence. So there’s no way to know for sure who had the first Delta case in the state, or to do contact tracing specifically for Delta-infected people.
It ‘hit the gound running’
But there are other ways to track the Delta variant’s spread in Missouri and elsewhere. Marc Johnson, a professor of molecular microbiology and immunology at the University of Missouri, is a kind of COVID-19 detective, tracking where and when variants are popping up around the Show-Me State by analyzing samples from sewersheds across Missouri on a weekly basis. (Sewersheds are land areas that share a common wastewater system, and can be a useful epidemiological tool.) While Johnson can’t identify the first people who carried the Delta variant in Missouri, he knows roughly where they used the bathroom. Wastewater can also be a predictive tool, because the coronavirus can shed genetic material in feces days before an infected person shows symptoms—or meets up with friends at a bar.
On May 10, Johnson’s team found the Delta variant in Missouri for the first time, in a sample taken from a sewershed encompassing the Ozark town of Branson. Branson’s population is only 11,000, but it’s a hotspot for concerts and other summertime amusements that draw more than 8 million visitors annually, according to the city’s Convention and Visitors Bureau. For Johnson, that meant one thing: the Delta variant was in Branson, but it wasn’t going to stay there.
Read more: The 6 Factors That Will Determine the Severity of the COVID-19 Surge in the U.S. This Fall
It’s just a theory at this point that Delta’s intrastate journey was fueled by people visiting and then leaving Branson. But the variant popped up in other sewersheds a week after his team first discovered it there, including up north in Linn County, where the virus “hit the ground running,” says Johnson. With a population of just 12,000, Linn has recorded 250 cases since the beginning of May, accounting for nearly a third of the total cases recorded there since the start of the pandemic 17 months ago.
“It was on national news how bad it was there,” says Johnson. “I was looking at whether that was going to be the same in other places. And it generally was. Almost everywhere where the Delta appeared—there was sometimes a delay, sometimes it was three weeks later—but then, pretty much without exception, it did eventually lead to this big increase.”

Given that the earliest upticks were happening in more rural and less vaccinated areas, Johnson initially thought that the virus was “picking and choosing” places to infect based on vaccination rates. But by early June, Delta appeared in more populated hubs like Springfield and Joplin, which have relatively higher vaccination rates—and local cases then ticked up.
The chart below shows all of the places where Johnson’s team is testing. Although the individual lines are hard to track, the trend is clear: once Delta rolls into town, it spreads fast, even in some places with relatively higher vaccination rates.
For example, Boone County, Missouri’s most vaccinated, is now reporting an average of 32.6 new daily cases per 100,000 people, compared with just 2.2 on Memorial Day. The city of Joplin had knocked its average daily count down to 3.4 cases per 100,000 in late March, but hasn’t dropped below 40 in the last month.
To Johnson, the spikes in even relatively highly vaccinated parts of Missouri are a reminder that, while the shots can reduce COVID-19’s severity, they can’t prevent 100% of infections. “People need to understand that the vaccines are extremely good at keeping people out of the hospital, at keeping people alive, but they’re not armor,” he says. “You can still be infected and can still infect other people. That doesn’t mean you can’t live your life, but if you don’t want to get sick, you can still use the easy precautions of wearing a mask if you’re in a crowded place, or avoiding indoor venues where people are screaming without masks on.” Indeed, the CDC’s newly revised mask mandate is based on thinking similar to Johnson’s.
Vaccinations are not keeping up
When COVID-19 vaccines started rolling out in the U.S. last winter, a pattern developed in Missouri, as it did elsewhere: each time the state expanded eligibility, eager people who were waiting to qualify would rush in. Then the numbers would drop off until eligibility expanded again. The last such bump was just after May 13, when people between the ages of 12 and 15 first became eligible.
But in early June, the number of people getting their first shot had fallen to levels not seen since the earliest days of the rollout, when supply was limited and appointments were hard to come by. In part, that’s because the virus appeared to be under control, reducing people’s sense of urgency. Missouri was at that point reporting fewer than 300 new cases a day, giving the appearance that the virus was being snuffed out—even though Delta was already circulating.
As the chart below shows, Missouri’s vaccinations are on the rise again. And this time, it’s not because of expanded eligibility—it’s because people who have been eligible for months yet remained on the fence are finally coming around, possibly out of fear of the Delta variant.
A closer look at the summertime uptick shows that people all over the state are now getting their first shots—including in places with lower vaccination rates and higher case rates. While that’s good news, it’s not entirely a reason to celebrate. Even given the recent uptick, the gap between Missouri’s most protected and least protected areas remains staggeringly wide; the counties with above-average case rates have lower initial vaccination rates than counties with below-average case rates had two months ago.
For now, Delta is hammering some pockets of the U.S., like Missouri and nearby states, far more so than others. But cases are rising across the country, suggesting we may be in the midst of yet another wave, especially in under-vaccinated areas. And when the virus is allowed to spread, it has an opportunity to mutate into new strains, which could prove even more capable of evading our vaccines. The Delta surge is also unlikely to die out before the school year, when millions of children—many of them unvaccinated—will be mingling together in classrooms. More and more employers, meanwhile, are demanding remote workers return to the office, though some are mandating vaccines or testing. With so many factors in flux, it’s impossible to predict how the U.S. Delta surge will play out. But if Missouri offers any lesson for the rest of the country, it’s that it’s far from time to let our guard down.
More Must-Reads from TIME
- Why Biden Dropped Out
- Ukraine’s Plan to Survive Trump
- The Rise of a New Kind of Parenting Guru
- The Chaos and Commotion of the RNC in Photos
- Why We All Have a Stake in Twisters’ Success
- 8 Eating Habits That Actually Improve Your Sleep
- Welcome to the Noah Lyles Olympics
- Get Our Paris Olympics Newsletter in Your Inbox
Contact us at letters@time.com