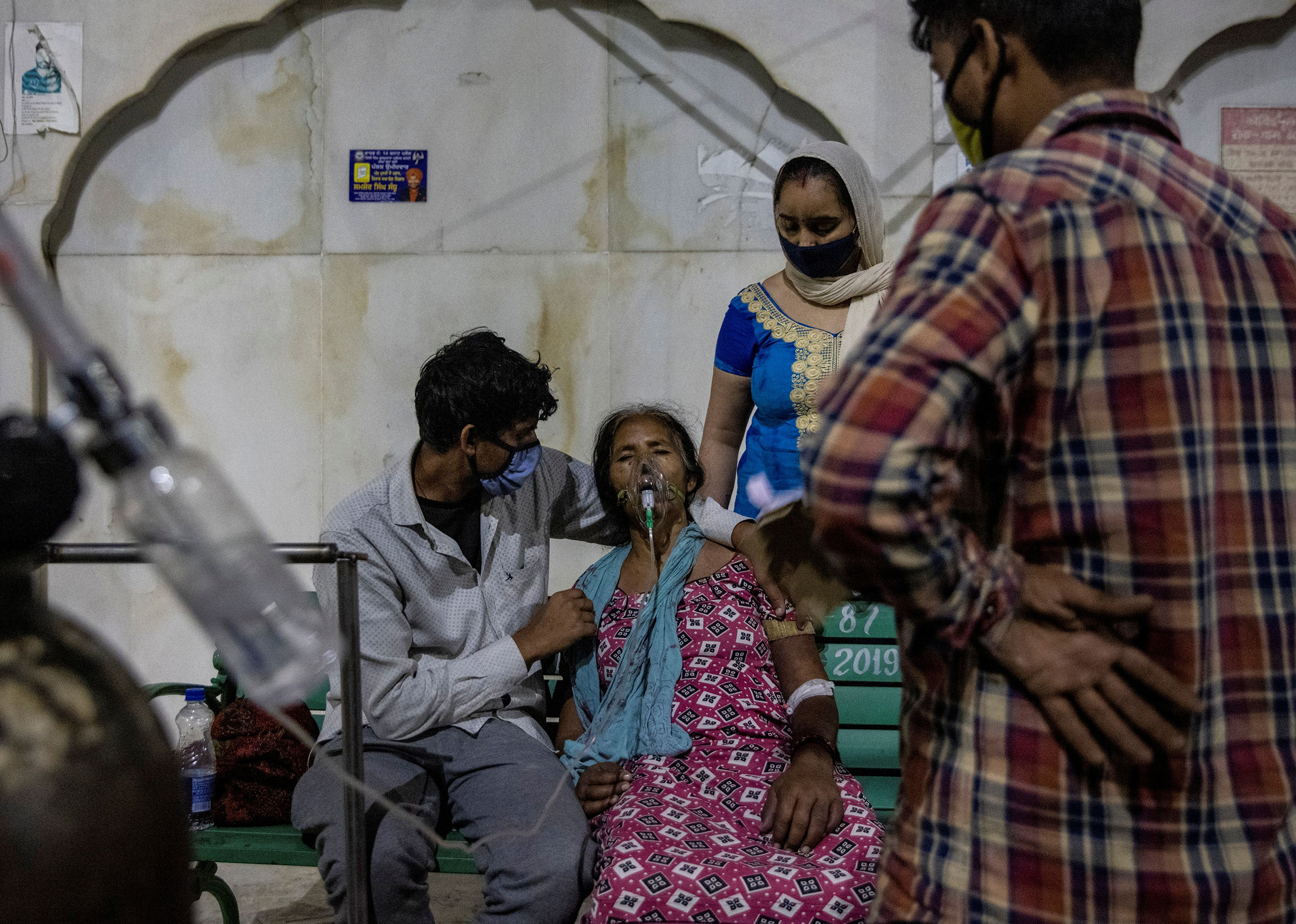
The pandemic won’t end for anyone until it ends for everyone. That sentiment has been repeated so many times, by so many people, it’s easy to forget it’s not just a cliche—particularly if you live in one of the wealthy countries, like the U.S. and Israel, that has made significant moves toward what feels like an end to the COVID-19 era.
Israel, for example, has fully vaccinated more than half of its population and about 90% of its adults 50 and older are now immune to the virus—enough that the country is “busting loose” and “partying like it’s 2019,” as the Washington Post put it last week. The U.S. is a bit further behind, with nearly 30% of its population fully vaccinated, but the possibility of a post-pandemic reality is already coming into focus. While daily case counts remain high, they are far lower than they were even a few months ago—about 32,000 diagnoses were reported on April 25, compared to daily tallies well above 250,000 in January. Deaths have also trended downward for most of 2021. The U.S. Centers for Disease Control and Prevention has relaxed its guidance on travel and indoor gatherings, and some states have repealed mask mandates and other disease precautions.
But while people in certain affluent countries celebrate a return to vacations and parties, COVID-19 remains a dire threat in many nations around the world—nowhere more so than India. For five days in a row, the country has set and reset the global record for new cases in a single day, tallying about 353,000 on April 26.
By official counts, about 2,000 people in India are dying from COVID-19 every day as hospitals grow overtaxed and oxygen supplies run short. Experts say the true toll is likely even higher than that. People are dying as they desperately seek treatment, and crematoriums nationwide are overwhelmed.
It can be difficult to grapple with that devastating reality when people in countries like the U.S. are reuniting with loved ones and cautiously emerging from lockdown. How can both scenarios be happening at once? The answer, as it often has during the pandemic, lies in disparity. As of April 26, 83% of vaccinations worldwide had been given in high- and upper-middle-income countries, according to a New York Times data analysis. In the developing world, many countries are preparing for the reality that it could take until 2022 or even 2023 to reach vaccination levels already achieved by richer countries today. Even in India, one of the world’s leading vaccine manufacturers, fewer than 10% of people have gotten a vaccine—a cruel irony, as people in India die in the streets while those thousands of miles away celebrate receiving their second doses.
To truly defeat COVID-19, we must reckon with that cognitive dissonance, says Dr. Rahel Nardos, who is originally from Ethiopia and now works in the University of Minnesota’s Center for Global Health and Social Responsibility. As an immigrant and global health physician who lives in the U.S., Nardos says she inhabits two worlds: one in which the U.S. may feasibly vaccinate at least 70% of its population this year, and another in which many countries struggle to inoculate even 20% of their residents in the same time frame.
“It’s a huge disparity,” Nardos says. “We need to get out of our silos and start talking to each other and hearing each other.”
That’s imperative, first and foremost because it could save lives. More than 13,000 people around the world died from COVID-19 on April 24. Remaining vigilant about disease prevention and monitoring, and working to distribute vaccines in countries that desperately need them to fight back COVID-19 surges, could help prevent more deaths in the future. That’s especially critical for developing countries, many of which are so overwhelmed by COVID-19 that nearly all other aspects of health care have suffered. “We may be looking at five, 10 years before they can get back to their baseline, which wasn’t that great to begin with,” Nardos says.
There’s also a global health argument for distributing vaccines more equitably. Infectious diseases do not respect borders. If even one country remains vulnerable to COVID-19, that could allow the virus to keep spreading and mutating, potentially evolving to such a point that it could infect people who are vaccinated against original strains of the disease. Already, vaccine makers are exploring the possibility of booster shots to add extra protection against the more transmissible variants currently circulating in various parts of the world.
We aren’t at that point yet; currently authorized vaccines appear to hold up well against these variants. But if the virus keeps spreading for years in some areas, there’s no telling what will happen, says Jonna Mazet, an epidemiologist and emerging infectious disease expert at the University of California, Davis.
“Evolution of those new strains could go into multiple directions. They may evolve to cause more severe or less severe disease. Some of the variants [could be] more concerning for young people,” Mazet says. “The whole dynamics of the disease change.”
And if the virus is mutating somewhere, chances are good it will eventually keep spreading in multiple areas, Mazet says. “Unless or until we have a major shift, we are still going to have large parts of every country that have a susceptible population,” she says. “The virus is going to find a way.”
The only way to stop a virus from mutating is to stop giving it new hosts, and vaccines help provide that protection. COVAX—a joint initiative of the World Health Organization; Gavi, the Vaccine Alliance; the Coalition for Epidemic Preparedness Innovations; and UNICEF—was meant to ensure that people in low-income countries could get vaccinated at the same time as people in wealthier ones. COVAX is providing free vaccines to middle- and low-income countries, using funds gained through purchase agreements and donations from richer countries. But supply and funding shortages have made it difficult for the initiative to distribute vaccines as quickly as it intended to. Many of the doses it planned to disseminate were supposed to have come from the Serum Institute of India, which delayed exporting doses in March and April as India focused on domestic vaccine rollout to combat its COVID-19 surge at home.
In the meanwhile, many poorer countries have been unable to vaccinate anywhere close to as many people as would be required to reach herd immunity. That will almost surely improve as new vaccines are authorized for use by regulators around the world, and as manufacturers scale up production, but those moves may be months away.
COVAX is also developing a mechanism through which developed countries could donate vaccine doses they don’t need. Some wealthy countries, including the U.S. and Canada, have contracts to purchase more than enough doses to vaccinate their entire populations, and have signaled their intent to eventually donate unneeded supplies—but timing is everything. That is, these countries will likely only donate once they are sure their own populations have been vaccinated at a level that ensures herd immunity.
On April 25, the Biden Administration said the U.S. would provide India with raw supplies for making AstraZeneca’s vaccine, as well as COVID-19 tests and treatments, ventilators, personal protective equipment, and funding. That’s a significant shift, since the export of raw vaccine materials was previously banned, but it still doesn’t provide India with ready-to-go vaccines. That step may be next, though. The U.S. will export as many as 60 million doses of AstraZeneca’s vaccine once the shot clears federal safety reviews, the Associated Press reports.
Gian Gandhi, UNICEF’s COVAX coordinator for supply, says he fears many wealthy countries’ vaccine donations may not come until late in 2021, just when global supply is expected to ramp up. That may cause a bottleneck effect: all doses may come in at once, rather than at a slow-but-steady pace that allows countries with smaller health care networks to distribute them. “We need doses now, when we’re not able to access them via other means,” Gandhi says.
The global situation is also critical now. Worldwide, more than 5.2 million cases and 83,000 deaths were reported during the week leading up to April 18. Indian hospitals are so overrun, crowds have formed outside their doors and desperate families are trying to source their own oxygen. Hospitals in Brazil are reportedly running out of sedatives. Iran last week broke daily case count records three days in a row. Countries across Europe remain under various forms of lockdown. Vaccines won’t change those realities immediately—but without them, the global community stands little chance of containing COVID-19 worldwide.
More Must-Reads From TIME
- The 100 Most Influential People of 2024
- Coco Gauff Is Playing for Herself Now
- Scenes From Pro-Palestinian Encampments Across U.S. Universities
- 6 Compliments That Land Every Time
- If You're Dating Right Now , You're Brave: Column
- The AI That Could Heal a Divided Internet
- Fallout Is a Brilliant Model for the Future of Video Game Adaptations
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Write to Jamie Ducharme at jamie.ducharme@time.com