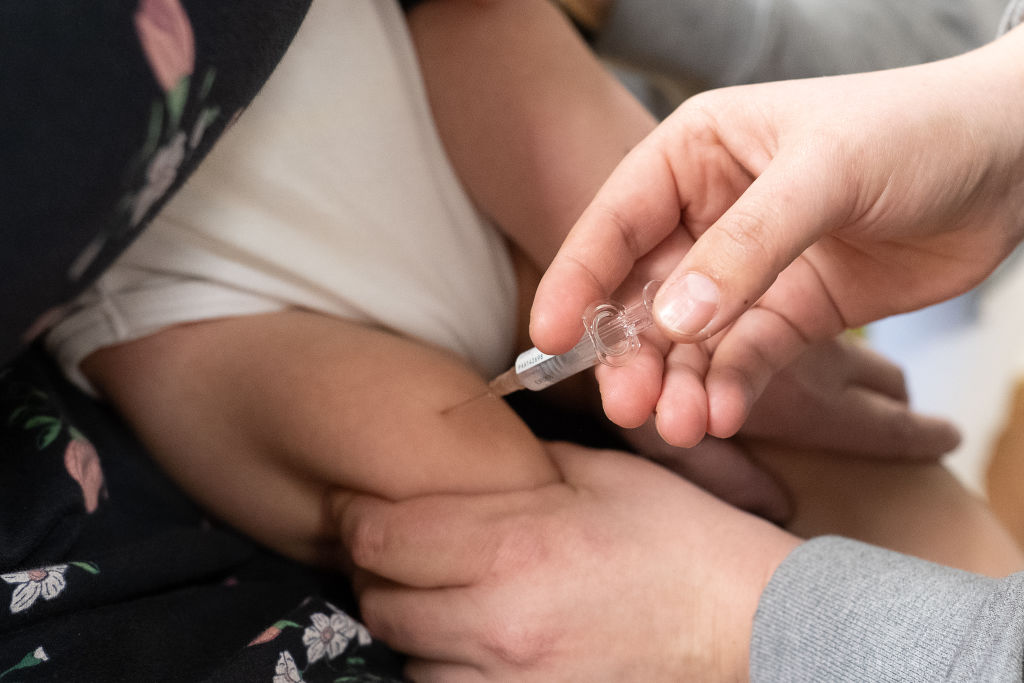
The world is entering a new era of vaccines. Following the success of COVID-19 mRNA shots, scientists have a far greater capacity to tailor shots to a virus’s structure, putting a host of new vaccines on the horizon.
The most recent arrivals are several new immunizations against respiratory syncytial virus, or RSV.
These shots are welcome since RSV can be dangerous, even deadly, in the very old and very young. But the shots, produced by Pfizer and GlaxoSmithKline, are also expensive, costing about $300 for those directed at adults, and up to $1,000 for one of the shots, a monoclonal antibody rather than a traditional vaccine, intended for babies. Many older vaccines cost pennies.
And in part because of the high cost, there is a shortage of RSV shots for infants, leading the U.S. Centers for Disease Control and Prevention to issue a warning for doctors to prioritize the most vulnerable babies.
More From TIME
The advent of these new drugs is forcing the U.S. to face anew questions it has long sidestepped: How much should an immunization cost that will possibly be given—maybe yearly—to millions of Americans? Also, given the U.S. is one of two countries that permit direct advertising to consumers: How can we ensure the shots get into the arms of people who will truly benefit and not those of people who seek it out as a result of scary marketing, at great expense?
Already, ads on television and the internet show active retirees playing pickleball or going to art galleries whose lives are “cut short by RSV.” This helps explain the lines for the shot at my local pharmacy.
The indiscriminate use of expensive shots could strain both public and private insurers’ already tight budgets.
The risk of RSV for infants
Other developed countries have deliberate strategies for deciding which vulnerable groups need a particular vaccine and how much to pay for it. The U.S. does not, and as specialized vaccines proliferate, public programs and private insurers will need to grapple with how to use and finance shots that can be hugely beneficial for some but will waste precious health dollars if taken by all.
A seasonal viral illness, RSV can cause hospitalization or, in rare cases, death in babies and in people ages 75 or older, as well as those with serious underlying medical conditions such as heart disease or cancer. For most people who get RSV, it plays out as a cold; you’ve likely had RSV many times without knowing it.
But RSV puts about 2% of babies under age 1 in the hospital and annually kills between 100 and 300 of those under 6 months, because their immune systems are immature and their airways too narrow to tolerate the inflammation. Merely having a bad case of RSV in young childhood increases the risk of long-term asthma.
Read More: Why it Took So Long to Get an RSV Vaccine
That’s why Dr. Barney Graham, the scientist who spent decades at the government’s National Institutes for Health perfecting the basic science that led to the current shots, said “the most obvious use is in infants,” not adults.
That’s also why a consortium of European countries, trying to figure out how best to use these vaccines without breaking the bank, focused first on babies and determining a sensible price. Though more of the very old may die of RSV, the years of life lost are much greater for the very young. (Babies can get the monoclonal antibody shot directly or gain protection through a traditional vaccine given to the mother near the end of pregnancy, conferring immunity through the womb.)
Examining the cost-utility of the vaccine, a team of European researchers looked at scenarios where the price was what the team termed “very expensive” —which they put at above €75 (about $80) – or “cheapish” which they put at below €25(about $27), says Philippe Beutels, professor in health economics at the University of Antwerp, who led the group.
While the calculus varies somewhat from country to country, the group concluded generally that if the price was at the high end, it was not cost effective. That meant, he said, “we should not give either kind of shot and stick to current practice” of treating sick infants—who usually do fine—with supportive care.
The calculation will be used by countries such as Belgium, U.K., Denmark, Finland, and the Netherlands to negotiate a set price for the two infant shots, followed by decisions on which version should be offered. “If the monoclonal antibody is €100 and the vaccine €10, then the vaccine would be preferable,” Beutels says.
They have not yet considered how to distribute the vaccines to adults—considered less pressing—because studies show that RSV rarely causes severe disease in adults who live outside of care settings, such as a nursing home.
Letting the market decide who gets drugs
Why did the U.S. focus first on older adults, while Europe is more concerned about RSV in infants?
In the U.S., the drug makers had a financial incentive: Roughly 3.7 million babies are born each year, while there are about 75 million Americans ages 60 and older—the group for whom the two adult vaccines were approved. And about half of children get their vaccines through the Vaccines for Children program, which negotiates discounted prices.
Also, babies can get vaccinated only by their clinicians. Adults can walk into local drug stores for the shots, and pharmacies are only too happy to have the business.
But which older adults truly benefit from the shot? Studies presented by the manufacturers to the U.S. Food and Drug Administration for approval in a population of generally healthy people 60 and older, so that’s the group to whom they may be marketed. And marketed they are, even though the studies didn’t show the shots staved off hospitalization or death in people ages 60 to 75.
Read More: How to Avoid the Tripledemic of Respiratory Diseases This Winter
That led to what some have called a “narrow” endorsement from the CDC's Advisory Committee on Immunization Practices (ACIP) for people 60 to 75: Patients in that age range could get the shot after “shared clinical decision-making” with a health provider.
In part because of this fuzzy, conditional endorsement, it is likely some Americans 60 and over with commercial insurance are finding that their insurers won’t cover it. Under Obamacare, insurers are generally required to cover at no cost vaccines that are recommended by the ACIP.
(In late September, the ACIP recommended immunization of all babies with either the antibody or the maternal vaccine. Insurers have a year to commence coverage and many have been dragging their feet because of the high price.)
A patchwork strategy
There are better and more equitable ways to steer the shots into the arms of those who need it, rather than simply administering it to those who have the “right” insurance or, swayed by advertising, can pay. For example, insurers, including Medicare, could be required to cover only those ages 60 to 75 who have a prescription from a doctor, indicating shared decision-making has occurred.
During the pandemic emergency, the federal government purchased all COVID-19 vaccines in bulk at a negotiated price, initially below $20 a shot, and distributed them nationally. If, to protect public health, we want vaccines to get into the arms of all who benefit, that’s a more cohesive strategy than the patchwork one used now.
Vaccines are miraculous, and it’s great news that they now exist to prevent serious illness and death from RSV. But using such novel vaccines wisely—directing them to the people who need them at a price they can afford—will be key. Otherwise, the cost to the health system, and to patients, could undermine this big medical win.
More Must-Reads from TIME
- Welcome to the Golden Age of Scams
- Introducing TIME's 2024 Latino Leaders
- How to Make an Argument That’s Actually Persuasive
- Did the Pandemic Break Our Brains?
- 33 True Crime Documentaries That Shaped the Genre
- The Ordained Rabbi Who Bought a Porn Company
- Why Gut Health Issues Are More Common in Women
- The 100 Most Influential People in AI 2024
Contact us at letters@time.com