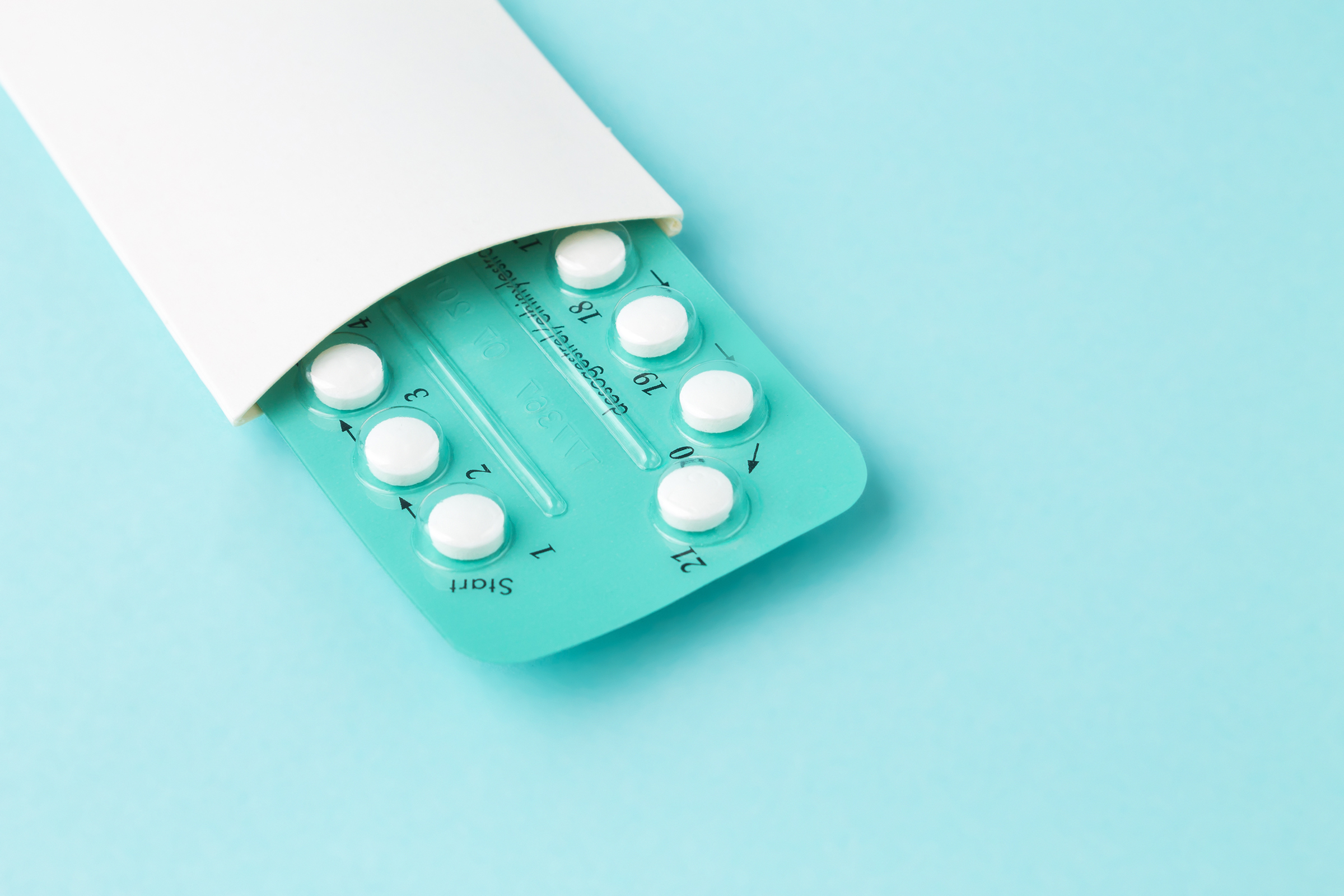
Since the Supreme Court overturned Roe v. Wade and set off a cascade of abortion bans around the country, access to contraception has taken on increased importance. To get birth control pills and other hormonal contraceptives in the U.S., patients still need a prescription. But now birth control pills are one step closer to being available over the counter.
HRA Pharma, a French drugmaker, has submitted an application to the U.S. Food and Drug Administration (FDA) for the first over-the-counter birth control pill in the U.S.
“We’re very proud of being the first company to submit the first-ever application to the FDA for daily birth control over the counter, and obviously it’s coming at the right moment,” says Frédérique Welgryn, chief strategic operations and innovation officer at HRA Pharma. Although the company had been working on its application for years before the Supreme Court’s decision, the announcement is “a bit of light in this very dark moment” for reproductive rights in the U.S., Welgryn says.
Nearly half of pregnancies in the U.S. are unintended, and research shows that nearly one third of women who have tried to access prescription birth control faced obstacles. If HRA Pharma’s application is approved, reproductive rights activists and researchers say an over-the-counter pill would remove barriers to health care and expand access to birth control throughout the country, especially for poor people, those in rural areas, and other marginalized communities.
Oral contraceptives were first approved by the FDA more than 60 years ago, and they are the most popular non-permanent method of birth control in the U.S. The pills are already available over the counter in more than 100 countries. And recent polling from Data for Progress shows that the majority of American voters across party lines support making birth control pills available without a prescription in the U.S.
More from TIME
In order for a medication to be sold over the counter in the U.S., the FDA says it must be safe, must treat a condition that users can self-diagnose, must have a low potential for misuse, and must be something people can effectively use without the supervision of a health care provider.
Many researchers and major medical associations in the U.S. say oral contraceptives meet all of the FDA’s requirements. Groups including the American College of Obstetricians and Gynecologists, the American Academy of Family Physicians, and the American Medical Association (AMA) have supported moving birth control pills over the counter for several years, and the AMA last month urged the FDA to approve over-the-counter access to the pills without an age restriction.
While millions of people take birth control pills every year and research has shown they are safer than pregnancy—which carries a higher risk of blood clots, among many other issues—there are some risks for people with certain medical conditions, which is why oral contraceptives have traditionally required a prescription. The vast majority of oral contraceptive sales are for pills that include both estrogen and progesterone, but HRA Pharma’s pill, called Opill, contains only progestin. Most progestin-only pills are not associated with an increased risk of blood clots, studies have shown, which may be part why HRA Pharma was the first company to be ready to apply with the FDA.
No company has previously submitted an application to the FDA to move its birth control pill over the counter. HRA Pharma has been working toward its application for about seven years. Another company called Cadence Health has been working with the FDA for about five years to ready an over-the-counter pill that contains both estrogen and progestin, according to a company spokesperson, and has not yet submitted its application.
There are likely several reasons that it’s taken years for pharmaceutical companies to get to this point, says Kelly Blanchard, president of Ibis Reproductive Health, a research and advocacy group that has worked closely with HRA Pharma. First, there has been an overall trend of large pharmaceutical companies reducing their investment in women’s health, and especially in contraceptives. The birth control market is made up of many generic drugs, so the products do not generate the kinds of large revenues that more specialized drugs can bring in. Most over-the-counter medications in the U.S. are also meant to treat acute symptoms rather than be taken on an ongoing basis the way birth control pills are, and drugmakers can be wary of trying new ideas. Finally, Blanchard notes that remaining stigma around sexual and reproductive health may have deterred some companies from pursuing an over-the-counter pill.
The FDA has said it aims to make a decision within 10 months once a company submits an application to move a drug from prescription to over-the-counter status, so HRA Pharma expects to know whether its pill is approved in the first half of 2023.
One remaining question will be the pill’s cost. It’s too soon to know the exact price, but HRA Pharma has started discussions with retailers, Welgryn says, and it plans to create a program that would offer financial assistance. “We’re committed to making the pill affordable for all those who need it,” she says.
While the Affordable Care Act requires that most health insurance plans cover all FDA-approved birth control methods without out-of-pocket costs, most insurers only cover birth control that is prescribed by a health care provider. (And even then, some health insurers have been denying coverage for birth control or imposing costs—an issue that congressional Democrats and the Biden Administration have recently sought to address as abortion access is curtailed around the country.)
Democrats in the House and Senate recently re-introduced legislation that aims to require insurers to cover over-the-counter birth control, and Ibis Reproductive Health plans to advocate for insurers to cover the new pill if the FDA approves it. “One of our key goals is to ensure coverage for over-the-counter contraceptives,” Blanchard says. The group has had some success expanding birth control coverage at the state level and plans to make the case to insurers and employers that they should cover an over-the-counter pill. “We are hopeful that we will move towards it being more common for insurance to cover it,” she adds, “because it’s really important for access and affordability that insurance does cover an [over-the-counter] pill.”
Still, while HRA Pharma’s application marks a significant milestone in birth control access in the United States, Welgryn emphasizes that even if the FDA approves their application, the pill isn’t a panacea. “We know that people need access to the full range of reproductive health care,” she says, “and that includes contraception, that includes abortion, that includes the whole range of what women need to control their reproductive life.”
More Must-Reads from TIME
- How Donald Trump Won
- The Best Inventions of 2024
- Why Sleep Is the Key to Living Longer
- Robert Zemeckis Just Wants to Move You
- How to Break 8 Toxic Communication Habits
- Nicola Coughlan Bet on Herself—And Won
- Why Vinegar Is So Good for You
- Meet TIME's Newest Class of Next Generation Leaders
Write to Abigail Abrams at abigail.abrams@time.com