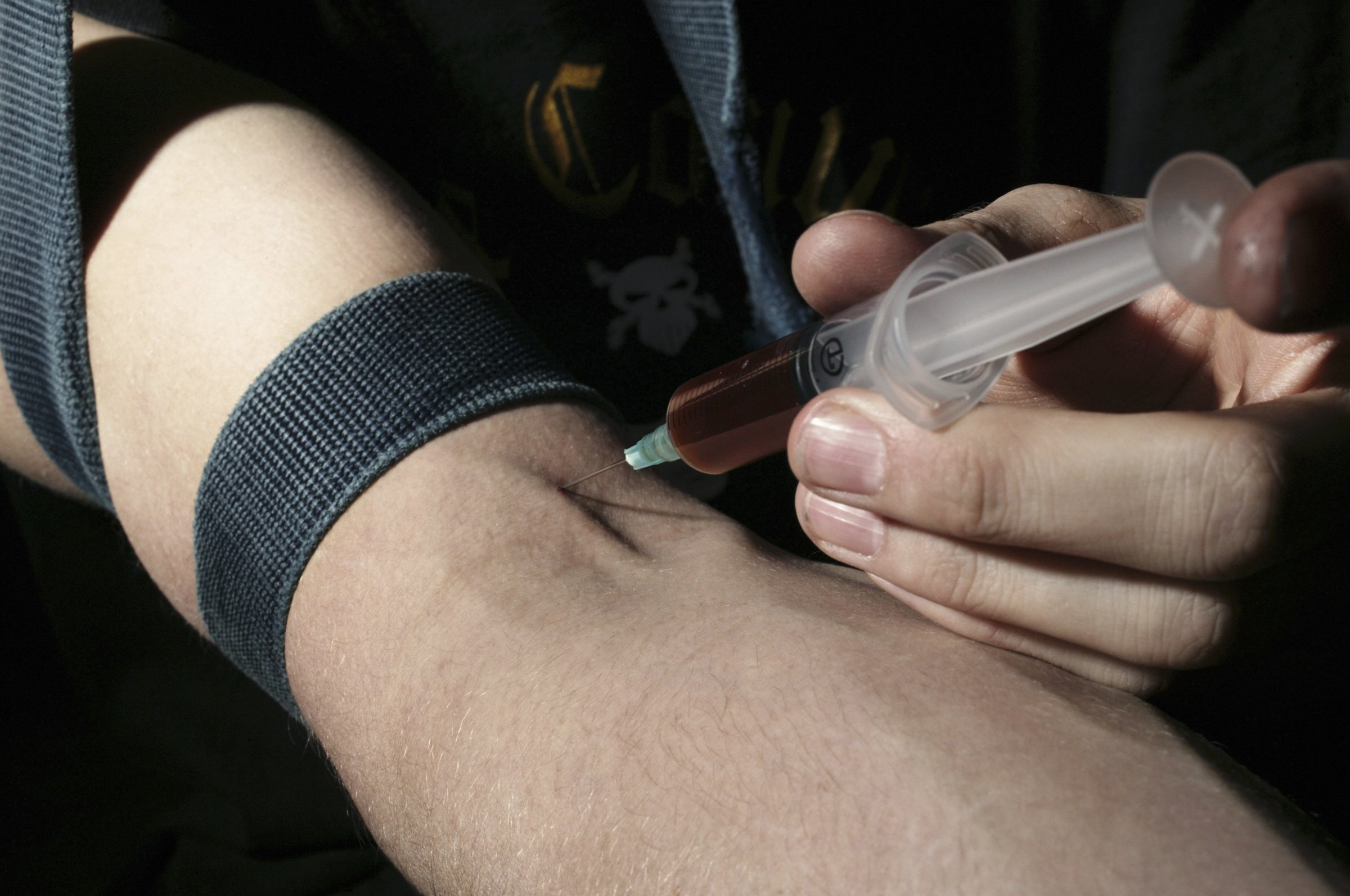
Every week, the chemist Kim Janda at the Scripps Research Institute gets at least one email—from an heroin addict or a person who loves a heroin addict—that goes something like this:
“I know you have no idea who I am, but I, as any true mother, want to save my son’s life—as does he! The problem is he can’t beat the craving and we are out of money. I will do whatever it takes to help him…Is there any way that he can become a part of a study for this vaccine?”
Janda responds to each email with the bad news that he has no current trials to enroll them, despite the fact that he has created what is likely the most promising vaccine against heroin addiction ever developed. Unfortunately, as is the case with lots of promising addiction research, no one wants to bankroll it.
“No pharmaceutical company is going to fund trials for heroin, no way,” says Janda, who’s been working on addiction vaccines for decades. “For meth? No way. Forget about it.” Janda has also worked on a meth vaccine. He has one for cocaine and one for a date rape drug too, but the heroin vaccine is the one he’s most confident about because it was proven to work a in clinical trials on rats. “The heroin one has been our best success in over 25 years of working—it’s the best data we’ve seen,” says Janda.
In 2013, preclinical trials of the drug on heroin-addicted rats showed those vaccinated didn’t relapse into addiction and were not hooked by high amounts of heroin in their system. “It’s really dramatic,” says Dr. George Koob, director of the National Institute on Alcohol Abuse and Alcoholism (NIAAA) who was involved in the heroin vaccine research. “You can inject a rat with 10 times the dose of heroin that a normal rat [could handle] and they just look at you like nothing happened. It’s extraordinary.”
Meanwhile, heroin addiction and overdose deaths are sharply increasing in the United States. A record number of people now use the drug, many of them “graduating” to heroin from painkillers. In July 2014, the CDC reported that 46 Americans die from an overdose of prescription painkillers every day. Doctors wrote 259 million prescriptions for pain killers in a single year—enough for every U.S. adult to have a bottle of pills. Painkillers and heroin both come from the opioid poppy, but heroin is considerably less expensive than painkillers and, while it’s illegal, it does not require a prescription.
“In the 60s and 70s, if someone was addicted to heroin, it meant they began by putting the needle in their arm,” says Dr. Andrew Kolodny, chief medical officer of the rehabilitation nonprofit Phoenix House. “That’s different from the average person using heroin today. It’s affecting mainstream, white America.”
The heroin vaccine, should it go to market, would not be the first pharmacological attempt to treat addiction. There are a handful of FDA-approved drugs like naltrexone and acamprosate for drug and alcohol addiction, and buprenorphine, which treats opioid addiction by curbing withdrawal symptoms. But they’re imperfect. For example, the medications must be taken every day, and stopping too quickly can also cause withdrawal.
Lack of funding for vaccine research aside, success has been elusive for the trials that have tested addiction vaccines on humans. A 2014 cocaine vaccine study showed disappointing results, and in 2011 a late-stage trial for a vaccine to help nicotine smokers fell short.
Such setbacks in the field hinder Janda’s own work and hopes at getting funding for his vaccines, he says.
Creating a vaccine for addiction is tricky because addictive drugs toy with the body and the brain, tapping directly into the brain’s reward systems, which are needed for survival. Vaccines have to interfere with that—without causing a number of other problems.
Janda’s vaccine works a bit like a sponge in the blood stream. If a person—or, in this case, rat—is inoculated, that “sponge” sucks up the drug and prevents it from reaching the brain. Some drugs for addiction will block receptors in the brain so when a drug reaches the brain it can’t activate it like it used to; the heroin vaccine prevents the drug from reaching the brain at all.
Janda and Koob are hoping to get investigational new-drug (IND) distinction from the FDA so that they can test the vaccine in humans. They have backing from the National Institutes of Health experts—National Institute of Drug Abuse allocated $27.1 million dollars to addiction-vaccine research in 2014—but it’s not enough for a human clinical trial.
Addiction vaccines are not without skeptics. Some experts think that the vaccine approach to addiction is small minded, since addiction is physical and psychological—and a vaccine would only treat part of the problem. Others cite earlier trials of other vaccines that didn’t pan out, such as a recent one for cocaine addiction. “I understand why there are skeptics,” says Dr. Andrew Kolodny of Phoenix House. “We have this expectation that for every kind of medical problem, there’s a perfect pill out there. But I think vaccines do hold tremendous promise for future treatments of addiction.”
If the heroin vaccine is to make it to human clinical trials, and even to market, it needs more research and the research needs more money. And while our understanding of addiction has evolved in recent years, many still view addiction as a moral failure of the addict, not something that can be cured or prevented using the same framework used for any communicable disease.
“I am not sure Americans realize that if they treated alcoholism and drug addiction they would save quadrillions of dollars in health care costs,” says Koob. “Go into any emergency room on the weekend and you will see half are there for alcohol and drugs. If for no other reason, investing in research on addiction will reduce health care costs in the future. That’s something I believe in.”
More Must-Reads From TIME
- The 100 Most Influential People of 2024
- Coco Gauff Is Playing for Herself Now
- Scenes From Pro-Palestinian Encampments Across U.S. Universities
- 6 Compliments That Land Every Time
- If You're Dating Right Now , You're Brave: Column
- The AI That Could Heal a Divided Internet
- Fallout Is a Brilliant Model for the Future of Video Game Adaptations
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Contact us at letters@time.com