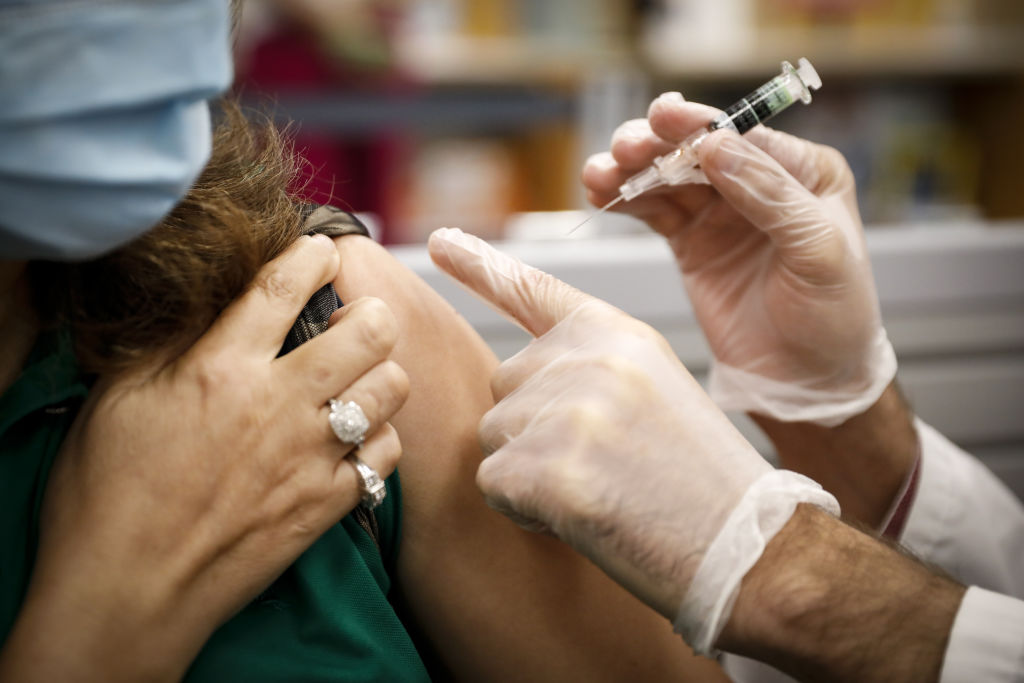
While the world awaits a proven COVID-19 vaccine, medical experts are turning their attention to a shot that’s long been a key component in the public health toolbox: the flu vaccine.
Experts hope this year’s flu shot can help prevent an influenza epidemic paired with another wave of coronavirus, which could overwhelm hospitals and lead to general confusion, given that it can be difficult to tell a COVID-19 infection from a case of the flu. This flu season is also something of a dress rehearsal for the eventual rollout of a COVID-19 vaccine amid the ongoing pandemic, allowing doctors, nurses and pharmacists a chance to get more people comfortable with the idea of a vaccine while also finding safe ways to inoculate people without spreading the coronavirus.
“While historically it’s fine to line [people] up and put them in close quarters—often in the winter, that’s inside—that’s not what we want to do here,” says Daniel Salmon, director of the Institute for Vaccine Safety at the Johns Hopkins Bloomberg School of Public Health. “So I think finding approaches and environments that are safe from a social distancing standpoint to vaccinate large numbers of people quickly—it’s absolutely an opportunity to get that right.”
Moreover, there are already data showing that people have mentally linked the flu shot with the coronavirus vaccine—suggesting that if public health officials can get more people to receive the former, those same people might be more likely to get the latter when it’s available. Abram Wagner, a research assistant professor at the University of Michigan’s department of epidemiology, recently conducted a yet-to-be-published survey of people from around the world, including 881 Americans, on their inoculation plans this August. He found that Americans who got a flu shot in the previous year were 363% more likely to want the flu shot again this year. More importantly, he found that those who received a flu shot during the last influenza season were 63% more likely to be planning to get the COVID-19 vaccine than those who did not.
Wagner says it would be understandable if some people wanted the flu shot but remained skeptical of the COVID-19 vaccine. After all, the flu vaccine, unlike those currently being developed for COVID-19, has been battle-tested over many decades (although it’s typically changed every year to counter the specific flu viruses expected to circulate in a given season). But people seem to be putting all vaccines in the same emotional bucket. “If you have experience with getting the jab, and you have the shot, it’s no big deal, then I think you will be just more likely to get another shot in the future, even if it’s not the same shot you got in the past,” Wagner says.
Influenza season in the northern hemisphere has only just begun, but there are some signs that the COVID-19 pandemic may be nudging more people than usual to get the flu shot. In an August survey of 1,000 people by the National Foundation for Infectious Diseases, 28% percent of U.S. respondents said the pandemic made them more likely to get the flu vaccine. Overall, 59% of people are planning to get the flu shot this season, the survey found, compared to 52% last season. (The U.S. Centers for Disease Control and Prevention estimates about 48.4% of American adults got the flu vaccine during the 2019-20 season, far short of the agency’s 70% target).
In terms of COVID-19, that 70% figure is also key—scientists think it’s generally about the amount of people in a given community that need to be immune to COVID-19 to reach herd immunity, depending on the vaccine’s effectiveness and the the strength of natural immunity through exposure. We may never reach that point. According to a Pew Research Center survey conducted in September, nearly half of U.S. adults said they probably or definitely would not get a COVID-19 vaccine—a sharp increase since May, when only 27% of Americans said they probably or definitely wouldn’t get the shot. That suggests faith in the eventual vaccine is quickly eroding, especially amid fears that it’s being rushed for political purposes.
Still, this year’s influenza vaccine rollout could help make Americans feel more comfortable about a possible coronavirus vaccine. For instance, medical practitioners could use a patient’s flu shot appointment to answer their questions about vaccines more broadly and make them more comfortable with the process, says Ann Philbrick, an associate professor at the College of Pharmacy and the Department of Family Medicine and Community Health at the University of Minnesota. Healthcare workers can provide “reassurance” about vaccines, she says, and “put the seed in your patient’s mind that we’re working on a COVID vaccine, and once we have one, it’s important to get one.”
More Must-Reads from TIME
- Why Biden Dropped Out
- Ukraine’s Plan to Survive Trump
- The Rise of a New Kind of Parenting Guru
- The Chaos and Commotion of the RNC in Photos
- Why We All Have a Stake in Twisters’ Success
- 8 Eating Habits That Actually Improve Your Sleep
- Welcome to the Noah Lyles Olympics
- Get Our Paris Olympics Newsletter in Your Inbox
Contact us at letters@time.com