People often talk about COVID-19 testing like it means only one thing. But in reality, the U.S. Food and Drug Administration (FDA) has so far granted emergency-use authorization to more than 200 different tests meant to detect a current or past infection from SARS-CoV-2, the virus that causes COVID-19. Most recently, the agency made headlines for approving the first such test that uses saliva samples, the aptly named SalivaDirect test out of the Yale School of Public Health.
These COVID-19 tests fall into three main categories: PCR, antigen and antibody. Dr. Aneesh Mehta, chief of infectious diseases services at Emory University Hospital in Atlanta, Ga., broke down the differences between them—and what to keep in mind if you decide to get tested.
PCR tests
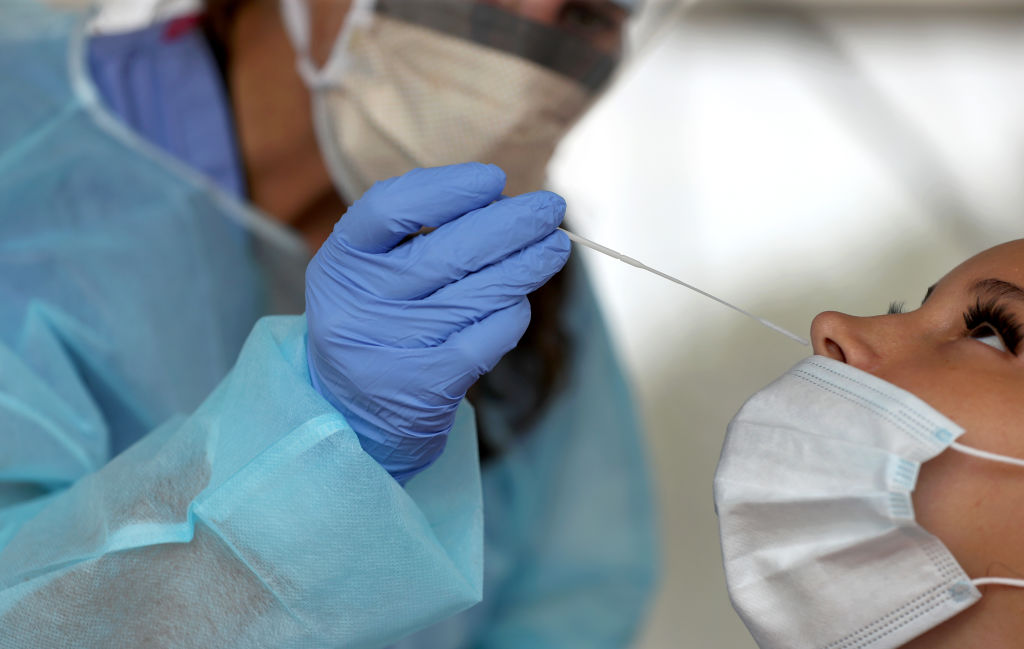
The majority of COVID-19 testing happening in the U.S. right now uses polymerase chain reaction (PCR) technology. These tests detect disease by looking for traces of the virus’ genetic material on a sample most often collected via a nose or throat swab. The U.S. Centers for Disease Control and Prevention (CDC) considers PCR tests the “gold standard” of COVID-19 testing, but, like all tests, they’re not perfect. Studies have suggested as many as 30% of COVID-19 PCR test results are inaccurate. (For comparison, the CDC in 2018 estimated that rapid flu tests have about the same rate of incorrect results.)
With COVID-19 tests, false negatives seem to be much more common than false positives—so if you get a positive result, you very likely do have the virus. If you get a negative result but have coronavirus symptoms or recently encountered someone sick with the virus, you should still self-isolate until symptoms subside.
False negatives can happen if health professionals do not go deep enough into the nose or throat to collect a good sample. The timing of the test matters, too. Infections can be missed if testing happens too soon after exposure, research shows. The reverse is also possible. “Sometimes after the virus has been killed off, there’s still a lot of [genetic material] left over in the body,” Mehta says. This can cause someone to test positive even if they’re not actively sick. Getting tested roughly five days after a possible exposure seems to be the sweet spot.
Running a PCR test and reading its results requires specific equipment and chemicals (known as reagents) that are in short supply, which is partially why the U.S. has hit such a testing backlog. To try to cut down on wait times, several companies have developed tests that can detect a virus’ genetic material in minutes, but some—like the Abbott ID NOW test used in the White House—have high reported rates of false negatives. These rapid tests aren’t readily available to most of the American public yet, but some experts argue they could serve a valuable purpose despite their questionable accuracy. Fast tests could significantly ramp up testing capacity, feasibly catching more cases of COVID-19 than our current testing strategy, despite the accuracy issues.
Saliva tests
Coronavirus saliva tests are a new type of PCR diagnostic for COVID-19. Saliva testing “does depend on standard PCR technology, and it does require some manual labor in order to move it through the steps of the test,” Mehta says. But collecting spit is less invasive than a nose or throat swab and easier to do at home or without medical training, Mehta says. SalivaDirect, the test from Yale, also does not require proprietary chemical reagents or test tubes, which its developers hope will help ease supply and access issues.
Early Yale research conducted by testing professional basketball players suggests the saliva test is about as accurate as a traditional nasal PCR test, but Mehta says “we need to more broadly test it” to see if that finding holds true.
Antigen tests
Antigen tests can turn around results in minutes—but speed comes with tradeoffs.
Like PCR tests, antigen tests usually require a nose or throat swab. But unlike PCR tests, which look for genetic material from the SARS-CoV-2 virus, antigen tests look for proteins that live on the virus’ surface. This process is a little less labor-intensive than PCR testing, since there isn’t as much chemistry involved, but it’s also less sensitive. Mehta says that opens the door for possible false positives (if the test picks up on proteins that look similar to those from SARS-CoV-2) or negatives (if it misses proteins entirely). False positives are rare with antigen tests, but as many as half of negative results are reportedly inaccurate. If you test negative but are showing symptoms or have had a risky exposure, your doctor may order a PCR test to confirm the result.
While antigen testing is becoming more common in the U.S., only a few such tests have been approved by the FDA so far. Much like with rapid genetic tests, some experts argue that fast-moving antigen tests could help ease testing bottlenecks enough to compensate for their reduced accuracy.
Antibody tests
Unlike the other tests listed here, antibody tests aren’t meant to pick up on current infection with SARS-CoV-2. Rather, they search the blood for antibodies, proteins the body makes in response to an infection that may provide immunity against the same disease in the future. These tests look for SARS-CoV-2-specific antibodies to see if you’ve previously had coronavirus.
Right now, antibody tests can’t do much except satisfy curiosity. For one thing, Mehta says, false results are fairly common. Even if the results are accurate, scientists do not yet know how well or for how long coronavirus antibodies protect someone from a future case of COVID-19. A positive antibody test result does not mean you can’t get COVID-19 again, at least as far as current science suggests.
Wide-scale antibody testing is useful for researchers, since it could inform estimates about how many people have actually had COVID-19 and help scientists learn more about if or how antibodies bestow immunity to coronavirus.
“From the research perspective, there’s a lot of information we can get from antibody testing if we collect it over time,” Mehta says. But in terms of actionable information for individuals, antibody tests don’t reveal much at this point. “Just because we can detect antibodies does not necessarily mean you’re fully protected from acquiring that infection,” Mehta says. “Continue to take all the same precautions that everyone else is taking.”
More Must-Reads From TIME
- The 100 Most Influential People of 2024
- Coco Gauff Is Playing for Herself Now
- Scenes From Pro-Palestinian Encampments Across U.S. Universities
- 6 Compliments That Land Every Time
- If You're Dating Right Now , You're Brave: Column
- The AI That Could Heal a Divided Internet
- Fallout Is a Brilliant Model for the Future of Video Game Adaptations
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Write to Jamie Ducharme at jamie.ducharme@time.com