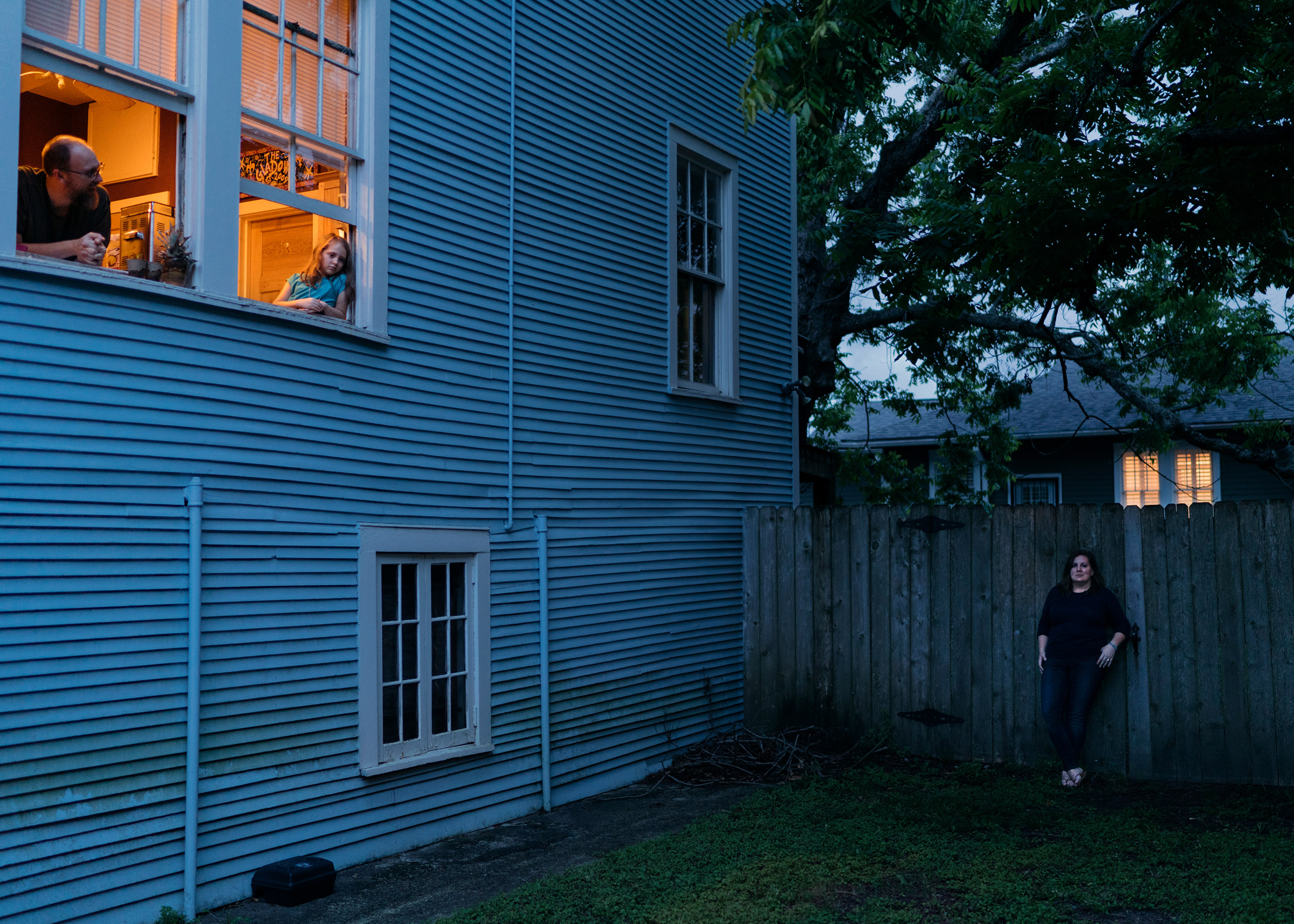
Driving around her Kearney, Missouri neighborhood is both respite and torture for Kathie Hodgson. She likes seeing other people out and about; it reminds her what life was like before COVID-19. But Hodgson, a 41-year-old teacher who lives alone after a recent divorce, says seeing happy families playing in their yards or walking their dogs can also send her plunging deep into a spiral of loneliness.
“You know, as much as I have valued my independence in the past year, it’s finally hitting me that I would like to curl up on the couch with somebody at night,” Hodgson says.
The irony, Hodgson says, is she was thrilled to live alone before the coronavirus pandemic hit, enjoying her “me time” and the newfound ability to date and see friends whenever she wanted—not long ago, she lived with her kids (who recently grew up and moved out) and a partner (who she recently divorced). But now that she’s confined to her apartment almost 24 hours a day, she is feeling the emptiness of her home acutely.
“Some days I smile and feel okay,” Hodgson says. “And other days I curl up in a ball and wonder if this goes on too much longer, will I be able to take it mentally? Can I last sanely living alone for months—a year?”
Even before the COVID-19 pandemic, public-health experts were concerned about an epidemic of loneliness in the U.S. The coronavirus has exacerbated that problem, with most face-to-face socializing for people still under lockdown orders indefinitely limited to members of their own households. For the 35.7 million Americans who live alone, that means no meaningful social contact at all, potentially for months on end.
Experts are rightly concerned about the mental health ramifications of this widespread isolation, especially since there’s no agreed-upon tipping point at which acute loneliness transitions into a chronic problem with long-term consequences. A group of doctors from Boston Children’s Hospital and Harvard Medical School warned in an April 22 commentary published in the Annals of Internal Medicine that physical distancing and stress caused by the pandemic, combined with rising firearm sales, could worsen the suicide crisis the U.S. has already been weathering for more than a decade.
On the other hand, some mental health advocates are optimistic that COVID-19 will finally give loneliness the mainstream recognition it deserves—possibly paving the way for a more socially connected future.
For such a common experience, loneliness is surprisingly slippery to define clinically. Loneliness is not included in the DSM-5, the official diagnostic manual for mental health disorders, but it goes hand-in-hand with many conditions that are. It’s often lumped together with social isolation, but the two concepts are different. Social isolation is an objective indicator of how much contact somebody has with other people, whereas loneliness is “the subjective feeling of isolation,” says Dr. Carla Perissinotto, a geriatrician at the University of California, San Francisco who studies loneliness. Being alone doesn’t necessarily mean you’re lonely, nor does being around people mean you’re not, Perissonotto says. Loneliness is a feeling only the person experiencing it can truly identify.
It can also be difficult to untangle whether loneliness is a symptom or a cause of a larger health issue: does someone withdraw socially because they’re depressed, or do they become depressed because they’re lonely? In any case, studies show chronic loneliness has clear links to an array of health problems, including dementia, depression, anxiety, self-harm, heart conditions and substance abuse. People without social support also have lower chances of full recovery after a serious illness than people with a strong network, studies show. The health consequences of loneliness are often likened to the effects of smoking 15 cigarettes a day—and far more common. While the most recent data show just 14% of American adults and about 5% of high school teenagers smoke cigarettes, a January report from health-insurer Cigna suggested around 60% of American adults felt some degree of loneliness, even before the COVID-19 pandemic hit.
Since lockdowns and stay-at-home orders were instated, roughly a third of American adults report feeling lonelier than usual, according to an April survey by social-advice company SocialPro. Another survey, also in April, for financial research group ValuePenguin, put the number even higher, at 47%. If the stereotype of a lonely person is a frail, elderly adult who lives alone, the coronavirus pandemic has exposed the truth that was there all along: anyone, anywhere, of any age can experience loneliness.
SocialPro’s survey of 1,228 people ages 18 to 75 predominantly living in English-speaking countries found that at least 20% of respondents from each age group polled were lonelier than usual as a result of coronavirus. Millennials were among the most likely age groups to feel lonely before COVID-19, research shows, and that’s no different now; 34% of millennials in the survey said they were “always or often” lonelier due to the pandemic.
Gender wasn’t a predictor, either: about 25% of women and 30% of men said they felt coronavirus-related loneliness. Nor does living situation necessarily dictate feeling. Caitrin Gladow, 41, has spent the last two months at home in New Orleans with her husband and three young kids—but she says she’s never felt more alone. She says she has zero emotional energy for self-care, since she’s juggling work, home-schooling and regular parenting while dealing with “paralyzing” stress and anxiety and the grief of losing people in her community to coronavirus. On top of that, she says, there’s the guilt for feeling overwhelmed when so many people are worse off.
“Even in a house full of screaming children who I love more than anything, I find that I feel especially vulnerable,” Gladow says. She feels an unspoken pressure “to be the glue of the family, and I’m trying not to let them down, but in the process I’m crumbling.”
And of course, elderly adults remain at high risk of loneliness. Given their susceptibility to serious COVID-19 infections, older adults are likely to be even more cut off from outside life. NORC at the University of Chicago found the coronavirus pandemic has made about a third of adults 70 and older lonelier than usual.
In other words, loneliness is everywhere, especially now. “This is a huge topic, but it’s been kind of sidelined,” Perissinotto says. “Now everyone is forced to look at this in a different way. We can’t keep ignoring this.”
Technology has emerged as an imperfect solution. Video-chat platforms like Zoom are surging in popularity, and nearly every social media network is billing itself as a way to stay connected with friends virtually. Instagram in March introduced a new feature that lets friends view posts together over video chat, specifically to foster bonding during COVID-19 isolation. Telecom companies like Samsung have donated smart devices to help people in quarantine stay connected.
There are also community groups attempting to make digital communication more meaningful. Some existed before COVID-19 but have expanded to meet surging demand, like Let’s Be Authentic, a Philadelphia-area social group that pairs up members for weekly video chats and communication exercises. It has seen a noticeable uptick in use of its online programs, a company representative says. And in Maryland, the state’s Department of Aging has adapted a program that provided daily automated wellness checks for seniors so that any elderly person who signs up also gets a personalized phone call from a volunteer at least once a week. “They know someone is there for them should they need it, and that alone makes you feel good,” says department secretary Rona Kramer.
Other groups have popped up in direct response to the crisis. A group of Cornell students built the platform Quarantine Buddy to match up users with similar interests for virtual conversations, and has so far attracted 8,000 people in 64 countries, ranging in age from 18 to 80.
But research suggests not everyone benefits equally from digital interactions. Several studies have found that tools like video chats and instant messages may help elderly adults feel less lonely, especially if they’re physically isolated from others and cannot otherwise socialize. But, interestingly, research shows that loneliness may subside for younger adults when they reduce their social media usage. In regular life, that may be because endless scrolling through other people’s social-media posts makes young people feel left out, or it may be because it’s replacing valuable in-person moments; under COVID-19 lockdown, social media may simply serve as a painful reminder of their loved ones’ physical absence. In ValuePenguin’s recent survey, 10% of respondents said video chats only make them feel lonelier.
Jessica Pflugrath, a 27-year-old freelance writer and editor who lives alone in Brooklyn, New York, has been relying on video chats to stay connected with her friends, but she says they bring a nagging feeling of unease. The ebb and flow of an in-person conversation doesn’t always translate to video, and she doesn’t like the pressure of having to be “on” all the time; she also doesn’t like how easily digital conversations lend themselves to distraction. “There’s a lack of feeling present with people, in general,” she says.
But with few other options available, people should probably make the best of virtual platforms, says Rudolph Tanzi, vice chair of neurology and director of the genetics and aging research unit at Massachusetts General Hospital. Stress related to loneliness can trigger inflammation in the body, he says, which in turn is linked to a host of chronic conditions. In the current context, social interaction is just as important for quelling that stress response as physical behaviors like getting enough sleep, exercising, practicing yoga or meditation, and following a balanced diet, he says.
“We use the term ‘social distancing’ but it’s completely the wrong term,” Tanzi says. “You want ‘physical distancing.’ That doesn’t exclude social interaction via some of these internet platforms.”
How much emotional benefit you get from virtual communication may come down to your mindset, says Jenny Taitz, an assistant clinical professor of psychiatry at the University of California, Los Angeles. “If we write off a friend texting us,” she says,”we’re not going to be able to enjoy or savor the dose of connection that they’re offering us.” Studies have shown that feeling socially supported can make a measurable difference for mental health, regardless of how much socializing you’re actually doing.
Christine-Marie Liwag Dixon, 30, has had years of practice communicating virtually. Most of Dixon’s family are in the Philippines, but she and her husband live in the New York suburbs, so extended family gatherings are rare. “I have more than a dozen cousins, and we’ve never all been in the same room,” she says. For years, Dixon has had to get by on small gestures of love, like a text or a picture of an especially good meal. That can be enough, if you frame it right, she says. “Even little, sporadic reminders like that remind us that no matter how far apart we are, even if we don’t see each other regularly…we still love each other, we’re still connected and we’re still a family.”
But for truly lasting change, the health care system also needs to buy in. A February report from the National Academy of Sciences, Engineering and Medicine concluded that health professionals should be screening seniors for loneliness, and entering warning signs into patients’ medical records just like any other condition. In the wake of COVID-19, that may become best practice for patients of all ages. The report’s authors also called on the government and health insurers to fund research into loneliness’ causes, effects and cures, and pushed for awareness campaigns about the scope of the problem among people of all ages. What can help now? Mindfulness training and cognitive behavioral therapy can be valuable anti-loneliness tools for people young or old, since reframing the way one perceives social support can make an appreciable difference in feelings of loneliness, Taitz says. And these techniques can be easily taught by a mental health professional over telehealth platforms, she adds.
At the very least, COVID-19 is making loneliness easier to talk about, which could encourage people who struggle with it to seek help or reach out to connections they do have, Perissinotto says. There’s a certain amount of stigma attached to any mental illness, but loneliness can be uniquely uncomfortable to talk about. It can feel like a personal failing to admit you don’t have the social network you want, and there’s a tendency for others to blame the victim, Perissinotto says. In one 1992 Personality and Social Psychology Bulletin study, for example, participants rated a fictional lonely person as less likable, social, competent and attractive than a non-lonely person. Experts hope that the fact that loneliness is now mainstream and easier than ever to talk about will finally change that perception.
Claire Lejeune, a 24-year-old photographer who lives in Los Angeles, says she’s not a lonely person by nature; her job, after all, involves being around people, and she’s active and social in her personal life. But when two of her roommates left her apartment to shelter in place elsewhere and the third began keeping mostly to himself, she says she found herself truly lonely for the first time she can remember—and somewhat uncomfortable with that realization.
“I’m privileged and I’m not doing as terribly as some people are in quarantine. I felt kind of bad to even say that I’m lonely because it’s like, ‘Oh, woe is she,’” Lejeune says. But when she decided to tweet about her feelings, she says she was met with a wave of support from people going through the same thing.
“There was definitely a sense of community within the loneliness,” Lejeune says. “Everyone can relate to it.”
More Must-Reads from TIME
- Why Biden Dropped Out
- Ukraine’s Plan to Survive Trump
- The Rise of a New Kind of Parenting Guru
- The Chaos and Commotion of the RNC in Photos
- Why We All Have a Stake in Twisters’ Success
- 8 Eating Habits That Actually Improve Your Sleep
- Welcome to the Noah Lyles Olympics
- Get Our Paris Olympics Newsletter in Your Inbox
Write to Jamie Ducharme at jamie.ducharme@time.com