If you ever end up in an emergency room, the first thing that happens is a doctor or nurse will check your “critical” vitals: your temperature, blood pressure, respiratory rate, and pulse. If those indicate your life is at risk, your care is prioritized over others who have already been waiting or who have been seen by a doctor but require additional testing (e.g. an x-ray or blood test) or a specialist to review their symptoms. This process, called “triaging,” is the global standard for allocating resources in emergency care.
Triaging is a marvel of modern healthcare if it is abundantly clear that you are on death’s door. But if there’s no textbook description of your condition, it can leave you needlessly suffering while the experts try to figure it out. That’s often the case for those with rare diseases, a group of conditions that are not individually common, but combined, affect an estimated 10% of the global population, some 475 million people. An estimated 80% of the 7,000 identified rare diseases are caused by DNA mutations that occur during pregnancy, meaning most of those with this category of illness are born with it. In many cases, these babies emerge from the womb with life-threatening conditions that doctors—working the triage system—will immediately address. However, this also tends to lead doctors to then ignore the underlying rare disease—an “unnecessary medical expenditure,” in the triage system framework.
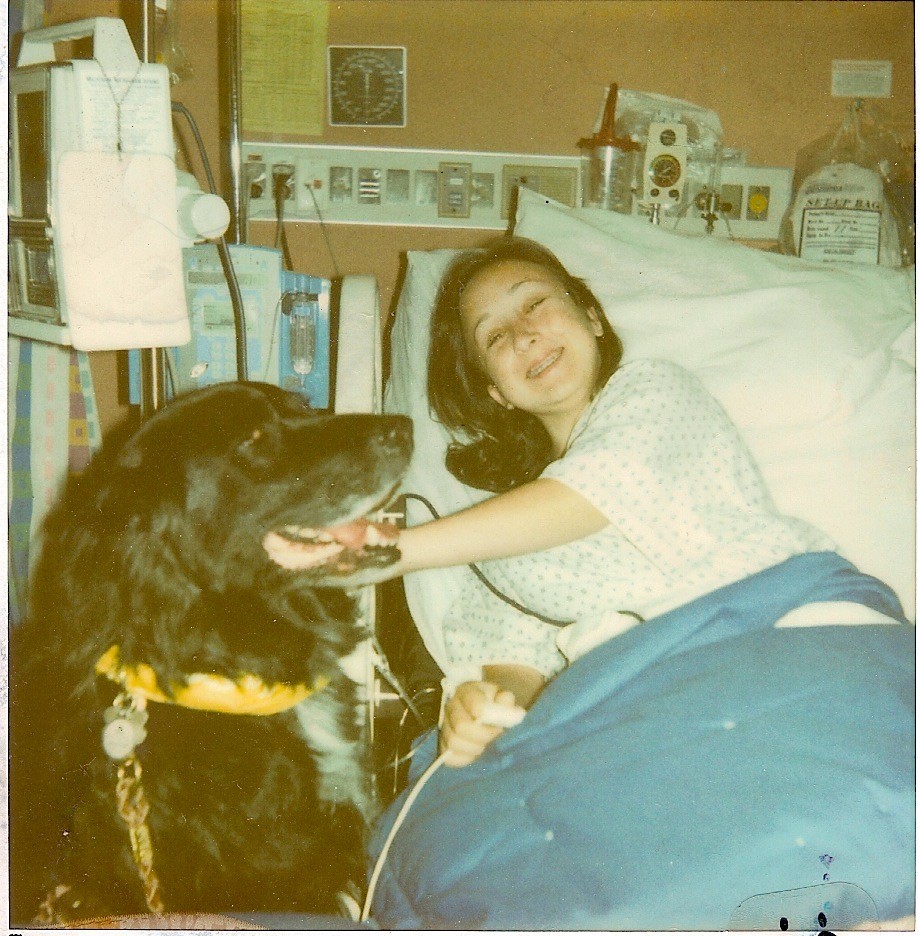
I am one of the people living with a rare disease.
I was born with a number of symptoms and signs that put my life at risk a collapsed lung, a premature exit from my mother’s body after only six months, and malnutrition from a hole in my amniotic sac. These problems were all treated and resolved over a multiple month stay in the hospital dictated by the triage system. I was allocated hospital resources for my life-threatening conditions until I was deemed stable enough to go home: the point at which I wouldn’t die if I left the care of the hospital.
But there was another problem that was overlooked, and which wasn’t diagnosed until I was five years old.
Every bone in my body was bent and every muscle atrophied or non-existent. I couldn’t move my neck away from shoulder; I couldn’t straighten my legs, knees, arms, wrists, ankles, toes, hands, or fingers beyond fixed, fully bent positions.
The triage system worked at saving my life, but never addressed how I would live day to day or even physically move from a single location by myself. It never addressed the underlying issue and root of the problem: a rare orthopedic genetic disease.
The “life or death” triage standard is one of the primary reasons that it takes, on average, seven years for people with a rare disease to get a diagnosis in the U.S.—and
I am one of the lucky ones. Serendipitously, a Because of these surgeries, and additional ones I’ve had since, I could feed myself, live free from a wheelchair, go to school through the post-graduate level, and hold a full-time job.
The orthopedic surgeries I needed—over 29 of them in less than 30 years—have cost millions of dollars. And these costs grow each year as I undergo additional exploratory surgery in the absence of any cure. However, these costs are still lower than what I would have incurred had I been left as the triage system deemed “stable” as an infant. I would have required 24-hour in-home care my entire life. I would never have been able to use the bathroom alone, to get dressed alone or to even leave the house alone. The lifetime value of a working individual according to the US Office of Management and Budget is on average $7 million to $9 million. The cost of a full-time caregiver is on average $40,320 a year; if a rare-disease patient reaches the average US life expectancy of 78 years old, the lifetime cost of full-time care is at least $3 million.
Our healthcare system needs to weigh the long-term costs of leaving behind people with rare disease, and, more specifically, evaluate the economic consequences that follow at a global scale.
Even more so, we need to weigh the costs of creating a pipeline to fill the treatment gap facing people with rare disease., Using genomic sequencing, clinicians can holistically understand the genetic roots of rare disease and even potentially cure rare disease through gene therapy, which modifies and permanently ‘fixes’ abnormal genes that cause a specific rare disease at birth.
Nonetheless, identifying the root genetic cause of rare disease is the only way to begin to cure a rare disease rather than just treating the symptoms in an ad hoc fashion. While certain pharmaceutical drugs can be developed from the findings in a genomic sequence to help mitigate or lessen symptoms, the science suggests the only way to cure a rare disease is to administer an even newer science called gene therapy—which modifies and permanently ‘fixes’ genes that are abnormal. Considered to be the most expensive option, a However, this nascent science is costly: gene therapy costs around $2 million for current US Food and Drug Administration (FDA)-approved options.
Insurance plans in the US rarely pay for clinical-grade whole-genomic sequencing (which can carry a price tag of up to $9,000)—let alone gene therapies. Yet if the most expensive cost to cure a rare disease is $2 million, that’s still far less than $3 million for a lifetime of full-time care (which excludes additional expenses). And new studies, like one the World Economic Forum released in the lead up to this year’s International Rare Disease Day, show that we can ultimately save money in the long term by funding more treatments and, as an added benefit, potentially develop more cures by learning when treatments work and when treatments don’t work.
We can’t create clinical pathways for the more than 7,000 rare diseases overnight, but we need a standard of care that goes beyond using death as the primary barometer of focus, over-simplifies the complexity of what it means to be “healthy,” and only considers short term costs. An economically effective, new model could center on allocating resources with the end goal to allow people to reach a level of health that provides basic mobility or basic independence—a level of health allowing economic productivity. We are living in a time of unprecedented medical innovation, and our system of coverage needs to catch up. We can do better than just keeping people alive.
More Must-Reads from TIME
- Cybersecurity Experts Are Sounding the Alarm on DOGE
- Meet the 2025 Women of the Year
- The Harsh Truth About Disability Inclusion
- Why Do More Young Adults Have Cancer?
- Colman Domingo Leads With Radical Love
- How to Get Better at Doing Things Alone
- Michelle Zauner Stares Down the Darkness
Contact us at letters@time.com