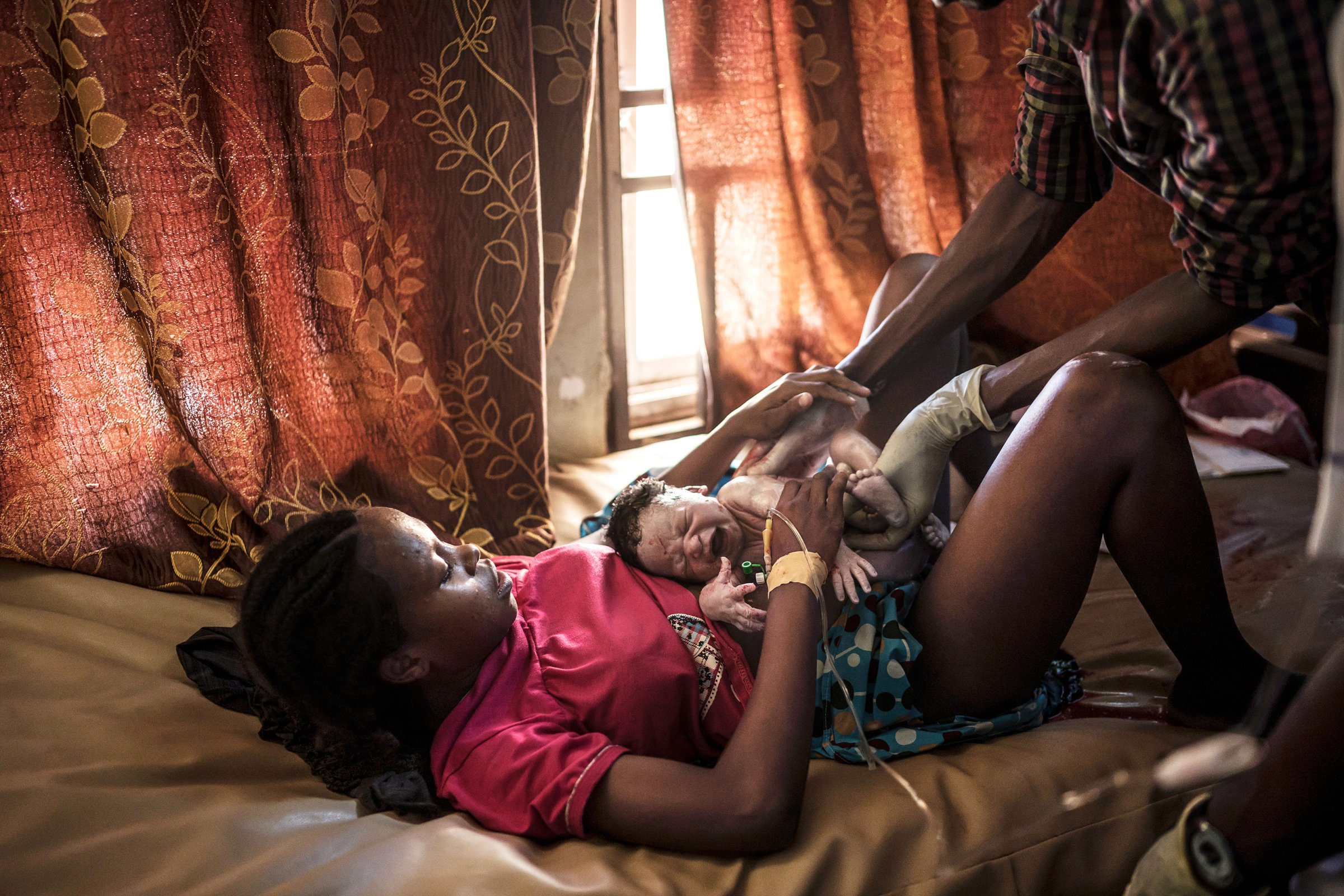
In the small, whitewashed medical clinic of Banki, one of northeastern Nigeria’s largest camps for internally displaced people (IDP), midwife Stella Aneto takes a rare pause between deliveries to catch her breath. Before wiping down the clinic’s sole delivery bed with disinfectant, Aneto glances at the clinic logbook. Two women have already given birth, and at least three others are in the early stages of labor. She instructs an assistant to prepare extra emergency supplies. Anything can go wrong when it comes to labor and delivery, but especially in a region with high rates of child marriage, malnutrition and malaria, where it’s not uncommon for midwives to tend to 18-year-olds giving birth to their fourth child.
In a bare-bones clinic that has no electricity or running water, and where the nearest hospital is 80 miles away, the chances of death in childbirth are extremely high. Yet Aneto hasn’t lost a single patient since she started working at the clinic 12 months ago. “I am always afraid of complications,” she says. “If something goes wrong, we don’t have what we need to help.” So Aneto’s goal is to make sure things don’t go wrong. And the only way to do that, she says, is to prepare. “Out here, preparing is our prevention.”
To read the full story, click here.
More Must-Reads From TIME
- The 100 Most Influential People of 2024
- Coco Gauff Is Playing for Herself Now
- Scenes From Pro-Palestinian Encampments Across U.S. Universities
- 6 Compliments That Land Every Time
- If You're Dating Right Now , You're Brave: Column
- The AI That Could Heal a Divided Internet
- Fallout Is a Brilliant Model for the Future of Video Game Adaptations
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Contact us at letters@time.com