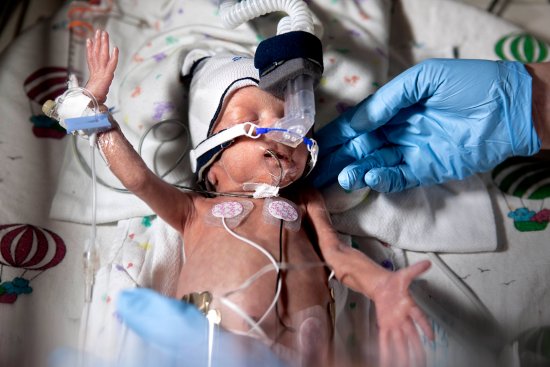
Dedicated caregivers are helping the tiniest babies survive—and thrive
It’s a safe bet that David Joyce knows more than you did when you were his birth age. That’s not hard, since what you knew back then was pretty much nothing at all. You knew warmth, you knew darkness, you knew a sublime, drifting peace. You had been conceived 29 weeks earlier, and if you were like most people, you had 11 weeks to go before you reached your fully formed 40. It was only then that you’d emerge into the storm of stimuli that is the world.
No such luck for David. He was born Jan. 28–well shy of his April 16 due date–in an emergency cesarean section after his mother had begun bleeding heavily. He weighed 2 lb. 11 oz., or 1,200 g, and was just 15 in. (38 cm) tall. An American Girl doll is 3 in. (8 cm) taller. Immediately, he began learning a lot of things–about bright lights and cold hands, needle sticks and loud noises. He learned what it feels like to be hungry, to be frightened, to be unable to breathe.
What all this meant was that if David wanted to stay alive, he’d have to work hard at it, and he has. Take drinking from a bottle–which he had never tried until a morning in late March, at the neonatal intensive care unit (NICU) of the Children’s Hospital of Wisconsin in Milwaukee. David had spent every day of his then seven-week life there, in the company of 58 other very fragile babies being looked after by a round-the-clock SWAT team of nearly 300 nutritionists, pharmacologists, gastroenterologists, ophthalmologists, pulmonary specialists, surgeons, nurses and dietitians and, for when the need arises, a pair of chaplains.
Under their care, he had grown to 18.1 in. (46 cm) and weighed 5 lb. 11.5 oz. (2,594 g), nourished by breast milk from his mother Melissa Hilger, 26, which was fed to him through a nasogastric tube threaded through his nose to his stomach. David’s father Kyle Joyce, 25, and Melissa live 90 minutes away in Randolph, Wis., where Kyle works as a diesel mechanic. They had been at the hospital every day after work for 51 days straight at that point–a three-hour round-trip–to spend a few more hours with David.
On that March morning, Merry Jay, David’s neonatal nurse, watched him until he stirred, then changed him and checked his monitor. His heart rate, respiration and blood-oxygen levels were good. Together, she and David waited for Katherine Fontier, a speech pathologist–which hardly sounds like a needed specialty in a NICU, but speech is all about the mouth, and today David was going to try to use his. Fontier arrived, checked the lighting (“When it’s too bright, preemies shut down,” she says) and gathered David into her arms, his lines trailing into his crib.
She dipped a pacifier into his mother’s milk and placed it in his mouth. His numbers stayed steady. She replaced the pacifier with a bottle filled with breast milk. David sucked, swallowing noisily. He squirmed, his heart rate and respiration dropped, and his blood-oxygen numbers flashed red. “He’s trying to coordinate sucking, swallowing and breathing,” Fontier said. She removed the bottle and gave him the pacifier. “O.K., O.K.,” she said softly. “Let’s go back to what he does well.” David got two more tries with the bottle that morning, then fell into an exhausted sleep. The feeding took 10 grueling minutes. In that span, he drank 2 cc of milk. A teaspoon contains 5 cc.
There was a time when David would not have stood a chance. According to government statistics, in 1960 the survival rate for infants under 1,500 g, or 3.3 lb., was 28%. In 2010 it was 78%, and a lot of that improvement has occurred just since the 1980s. The survival for any one baby is dictated first by the calendar. Come into the world at 22 weeks and you have only a 5% chance of making it out of the hospital alive. The odds improve to 26% at 23 weeks, 56% at 24 weeks, 76% at 25 weeks and up into the high 90s at 32 weeks and beyond. Even then, the battle’s not won, since the longer a baby remains in the womb, the fewer health problems there will be later. Still, survival is the first goal.
“Every decade since the 1960s, the age of viability has been reduced by a week,” says Dr. Edward McCabe, medical director of the March of Dimes Foundation.
This kind of progress inevitably raises tough questions. If you can keep a 22-weeker alive, what about 21 weeks, 20 weeks? How low is it fair to go if survival means a lifetime of prematurity-related disabilities? Seventeen percent to 48% of preterm babies, for example, will have some kind of neuromotor abnormality, including cerebral palsy. Cost is another issue. The March of Dimes calculates that babies born before 32 weeks’ gestation run up an average hospital bill of $280,811. Other estimates are lower, but either way, preemie care isn’t cheap. How much of a burden on a family–and suffering by a baby–makes sense?
Fortunately, for most preemies things are not this dire. Thanks to advances that had not been made even a few years ago, the odds of surviving and thriving are improving all the time. Lives that once might have begun and ended in a NICU can now be lived long and well–and there are many reasons that’s true.
Medical Mission Control
The biggest change in the care of preemies occurred very recently–in the past two years, in fact. For a long time, the most sophisticated of the newborn facilities was known as a Level III NICU, which was supposed to be equipped with all of the surgical capabilities and subspecialists needed to handle the tiniest and sickest babies. But there was no consistent policing of the standards for a Level III designation, so survival could be a geographical crapshoot. A preemie born within an ambulance ride of a good Level III would have a better chance of surviving than a same-size baby born elsewhere.
In 2012 the American Academy of Pediatrics decided to set that right, calling for the formalization of the standards applied to all three levels as well as the creation of a new Level IV designation for NICUs that not only have the staff and ORs to handle the toughest cases but are centrally located and can gather in families from the largest geographical footprint possible.
Competitive hospitals acted fast, and many have already made the changes necessary to earn a Level IV certification from their state hospital boards. The national numbers are still very murky, and for a lot of reasons: the states don’t all talk to one another, no single body serves as a clearinghouse for Level IVs, and some states are still working from the old designation of Level IIIc, which might be a IV in a different jurisdiction. However, the trend is promising, especially in big cities. Denver, Seattle, New York, Chicago, Atlanta, St. Louis, Philadelphia, Dallas, Boston and others have all cut ribbons on Level IVs, and many cities have more than one.
“There is so much that can go wrong with these babies so fast,” says Dr. Michael Uhing of the Milwaukee Level IV that was home to David. “You don’t have any choice but to come at the problem with as big a team and as many options as possible.”
Uhing’s NICU is among the best of the new breed, with a 97.5% discharge rate for preemies in the 2.8-to-3.3-lb. range (1,251 to 1,500 g) and a patient population that comes from across Wisconsin and four surrounding states. Kyle Joyce and Melissa Hilger are typical of the parents of those babies, living in a community that has a perfectly fine hospital but not one with a Level IV facility–and suddenly needing one. “We had just finished painting David’s room, and the next day I was in the [local] ER,” Melissa says. “The room is still a work in progress.”
The ER led to the Milwaukee NICU, and Kyle and Melissa had to get used to the fact that it was a place they were going to come to know well. The average preemie is not released to go home until what would have been the 37th week of gestation, which meant months for a 29-weeker like David. (He was actually released on April 17, one day past his 40-week, full-term due date.) Making things worse, from the moment parents arrive, the baby’s care is taken out of their hands. For the mother, nursing and pumping milk help some–it’s the one thing that only she can do. For the father, excluded from that loop, things are harder. “I’m a mechanic,” says Kyle. “I’m supposed to be able to fix anything. But I can’t fix this.”
The three-shift, 24-hour workday in the Milwaukee NICU begins with a morning meeting dubbed “the huddle,” during which Uhing and the team gather to review the status of each baby. There is a quick, round-the-horn quality to the gathering, and that is by design. “The huddle is conducted standing up,” says Sarah Currie, a nurse and patient-care manager. “It gets the doctors to the babies as quickly as possible.”
What awaits them changes every day. On the morning David struggled to drink his milk, Uhing and his team met a newly arrived family. Around the 27-week-old baby’s incubator-like isolette, the lights were dimmer, the thicket of poles, drips and monitors denser. The little girl was born with a contraction of the limbs caused by moving too little in the womb, which can be linked to a neurological anomaly, though no one could know for sure until she was stable enough for a brain scan.
Even as this visit was under way, word came that another pretermer–a boy–was being born in the hospital. By the afternoon, the baby had arrived in the NICU, and it was clear that there was not just the possibility of neurological anomaly; there was grave brain damage from which recovery was unlikely. The mortal calculus is always relative in the NICU. Almost every set of parents can look around and find a family they envy and a family they ache for. The only families no one wants to be are the ones whose babies are never going home.
The team’s visit to David’s crib was happier, not least because of the very fact that it was a crib. “We don’t want our preemies burning calories to stay warm,” says Currie, “so we keep them in an isolette to balance their temperature until they’ve put on weight. David graduated to a crib a couple weeks ago.”
Uhing reviewed David’s growth chart, and it looked steady, but he reminded the residents that growth isn’t everything. “We used to try to send home chubby kids,” he says. “Now we like them lean and mean. If the only goal is getting calories into them, we may set them up for obesity later.”
The Care Cascade
The mere fact that something can go wrong with as straight-up a treatment as getting food into a baby who badly needs it only hints at the complex, interlocking problems that preemie care involves. When it comes to the digestive system, overfeeding is just one complication. A preemie’s gut is not yet fully up to digesting anything, including breast milk, and the combination of inflammation, bacteria and low oxygen levels can cause infection; that, in turn, may lead to necrotizing enterocolitis, or tissue death in the intestine. What determines which babies will develop the disorder is a mystery, however. “Some sail through, while others have problems,” says Dr. Ganesh Konduri, a Milwaukee neonatologist. “But they all look the same when they come in.”
Milk and medications can work against each other too. Preemies are administered medicine in vanishingly tiny doses–little more than the residue that would be left in a syringe or IV line after an adult dose is given. The only way to make sure all the medicine is taken is to mix it with some carrier fluid. But the fluid may dilute the effect of hard-won feedings, and every drug has a different chemical interaction with milk. For that reason, there is a constant negotiation between pharmacists and dietitians during the morning huddles and the weekly staff meetings at which every case on the ward is reviewed.
“I have to stay on good terms with the pharmacists,” says dietitian Elizabeth Polzin. “I say what I want, and they tell me if it’s safe. ‘If you want more protein, you’ll have to cut down on something else.’”
Getting preemies to breathe is far more complex, with far more danger of downstream effects. Preemie lungs lack mature air sacs–or alveoli–in which the exchange of oxygen for carbon dioxide takes place, as well as the production of a substance known as surfactant, which prevents the lungs from collapsing and helps them absorb air and reject water. Artificial surfactant, administered into the trachea, was approved in 1990 and by 2002 had reduced deaths from respiratory distress in babies fifteenfold. That plus respirators, cannulas (nasal prongs that steadily feed a baby air) and the use of constant passive airway pressure (CPAP)–similar to the masks adults with sleep apnea wear–usually allow babies to absorb enough oxygen. David wore a CPAP for the first 17 days of his life, which was hard for the family. “It was such a high moment when he got rid of it,” says Kyle. “We could see his face for the first time.”
Even for good breathers, oxygen comes at a price. The highly reactive oxygen ions known as free radicals can scour lung tissue that’s already under siege. In the wrong quantities, oxygen can also lead to excessive blood-vessel growth in the eyes, damaging the retina and leading to what’s known as retinopathy of prematurity (ROP). It’s ROP that cost Stevie Wonder, born prematurely in 1950, his sight. “It’s amazing that we’ve been doing neonatology for so long and still don’t know what the oxygen level should be,” says Uhing.
The least predictable consequence of treatment involves the preemie brain. Even a quiet NICU is a too cold, too bright assault, and much of the bustle is uncomfortable or painful. A 25-week-old baby is not meant to have a tube down its throat, a needle in its arm and monitors taped to its skin. Every one of those sensory insults takes a toll. “The brain doesn’t develop the way it should,” says Konduri. “MRIs show significant differences between a full-term baby and a 40-week baby who was born prematurely.”
Fixing the Problems
While the 37-week guideline is the broad rule for how long any one preemie will remain in the NICU, innovative treatments are being developed to get all preemies home sooner and stronger. One of the most powerful–and newly appreciated–therapies is as old as the human species: just plain holding babies as much as possible, a technique called kangaroo care.
It’s no accident that infants are hardwired to need cuddling and adults are hardwired to love to oblige. Respiration, heart rate, sleep cycles, appetite and more stabilize when a baby is in an adult’s arms. Oxytocin–the hormone often called the cuddle chemical–rises in both the cuddlee and the cuddler. And when that cuddler is the mother, the extra oxytocin finds its way into breast milk, which doubles down on the dose the baby gets.
A newly released Israeli study followed a group of NICU babies born in the late 1990s, some of whom got kangaroo care and others who did not. At that time, the technique was not considered standard treatment and hospitals didn’t provide it on a systematic basis–at least not one that went beyond the amount of holding the babies received when relatives came to visit or they were otherwise being tended to. During exams at 3, 6, 12 and 24 months as well as at 5 and 10 years, the children who got constant cuddling outperformed the other group, with stabler sleep patterns, steadier respiration and heart rates and better attention skills.
For all that, even a preemie’s mother may find holding her baby surprisingly difficult, something Shannon Dreier, a Milwaukee mom whose son Abram was born at 26 weeks of gestation, discovered. “I was afraid to touch Abe,” she says. “The nurses are used to these babies. They’d say, ‘Get your hands in there.’ But it wasn’t until about a week after he was born that I was able to do kangaroo care.”
Another new treatment, far more experimental, involves the use of inhaled nitric oxide to increase blood flow to the lungs and improve function. The molecule–which is different from nitrous oxide, or laughing gas–is a vasodilator and is what helps give erectile-dysfunction drugs the power to do what they do. For now, nitric oxide is delivered to preemies as a gas in low concentrations–about 10 parts per million–and is used only in babies who badly need it, because while it may benefit the lungs, its effect on other organs is less certain. Harry Ischiropoulos, a biochemist at the Children’s Hospital of Philadelphia (CHOP), home to a celebrated regional NICU that is known for its research wing, is conducting studies to determine the impact of nitric oxide on brain metabolism, neurotransmission and responses to inflammation. “Nitric oxide may give a boost to neurotransmitters,” Ischiropoulos says. “That could benefit the brain as a whole.”
Investigators are also looking into ways to bolster the preemie’s immune system in hope of reducing infections and inflammatory diseases, particularly colitis. One way could be probiotics. A premature baby can be overwhelmed by some pathogens it finds in the outside world. But strategic dosings with beneficial bacteria may help the immune system switch itself on and get itself moving. “We could make a cocktail to administer to babies to rebuild the gut in the right way,” says Dr. Scott Worthen, a CHOP physician and investigator.
Other research involves pinpointing genes in the mother that may contribute to premature birth as well as those in babies that determine who will suffer complications and who won’t. Ophthalmologists at CHOP are investigating drugs to inhibit abnormal blood-vessel growth in the eye and prevent loss of vision. Currently, laser surgery can control the problem, but it’s more invasive and often not an option at all in the developing world. “Kids are going blind, and we know what to do about it, but we don’t have the resources,” says ophthalmologist Graham Quinn.
Endgame
Surviving babyhood is only part of the struggle. Premature babies have a lifelong higher risk for a whole range of problems. The odds of intellectual disability among preemies increases anywhere from 1.4-fold to 22-fold, depending on gestational age and birth weight. Stanford University researchers recently found that people born prematurely stand a 38% greater risk of dying in young adulthood than full-termers, typically from heart problems, though the absolute numbers–fewer than 1 in 1,000 deaths–put that danger in perspective. University of Rhode Island studies found a 32% greater risk of asthma and vision problems. Overall, about 66% of preemies born before 27 weeks have some kind of disability at age 3, and many never fully recover.
Some, of course, don’t even get that far. Nearly all the progress in survival rates in the past 30 years has come from improving the outlook for babies born past 23 weeks. Below that, the numbers have barely budged. “You get to the point that the lungs are so immature, you’d need entirely different treatments,” says Uhing. “The skin is like a burn patient’s. It just falls off.”
The job in these cases is much more straightforward: to keep the baby comfortable and prepare the family for what is to come. Milwaukee teaches nurses how to make plaster foot molds of the babies while they’re still alive. Those keepsakes are added to a memory box that includes the baby’s first–and sometimes only–swaddling blanket and T-shirt, as well as a family photo. And while babies in intensive care are kept in as isolated and germ-free an environment as possible, when the game is lost and everyone knows it, the rules are waived.
“Some parents want to take the baby outside to see the stars or feel the sun at least once,” says Currie. “The lifesaving piece no longer applies.”
More and more, however, the life is saved, the baby does come home, and there are plenty of sunny days and starry nights ahead. In some ways, the work of a NICU will always seem like an exercise in disproportion–an army of people and a mountain of infrastructure caring for a pound of life. But it’s a disproportion that speaks very well of us. The babies, increasingly, are reaping the benefits.
