Before this year, polio didn’t feel like an urgent threat. The disease was eradicated in the U.S. in 1979, and thanks to a global vaccination campaign, it’s endemic (though far from widespread) in just two countries—Pakistan and Afghanistan.
But the calculus changed in 2022. In July, an unvaccinated man in New York state contracted polio. And this year, poliovirus has circulated in wastewater in London, Jerusalem, and—as recently as Oct. 28—in New York City and several surrounding counties. “Unvaccinated and undervaccinated in these areas are at risk for paralysis disease,” researchers wrote in a report announcing the new New York findings. Anyone who falls into that category “should complete the vaccination series as soon as possible.”
Paradoxically though, one of the two types of polio vaccines is playing a role in the recent spread. To combat the outbreak, the U.S. government is considering rolling out yet a third variety of vaccine. Here’s what you need to know about the two different polio vaccines, the new one on the horizon, and how to keep your family safe.
The differences between the two polio vaccines
The first polio vaccine, developed by Dr. Jonas Salk and approved in the U.S. in 1955, is known as the inactivated polio vaccine (IPV). It is administered by injection and uses a killed poliovirus to familiarize the immune system with the disease and prime it to recognize a live, wild virus should it ever encounter one.
The second, developed by Dr. Albert Sabin and approved in the U.S. in 1963, is known as the oral polio vaccine (OPV) and uses an attenuated—or weakened—strain of the virus: one that can’t cause disease but can do the same job of priming the immune system as the IPV.
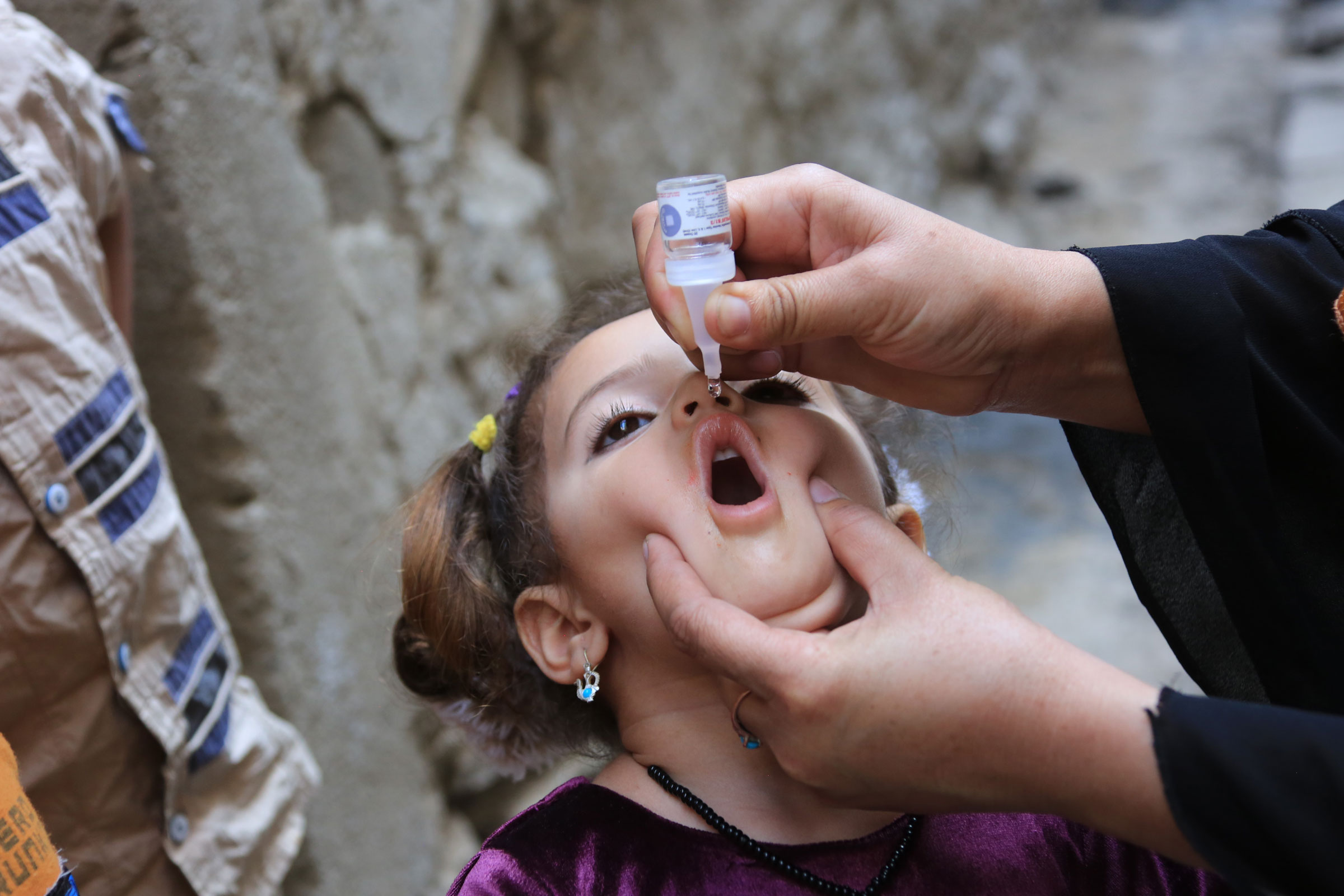
The OPV has two big advantages: it’s easier and cheaper to administer—with just a few drops to the tongue—than the IPV. That’s why it has been the vaccine of choice for the Global Polio Eradication Initiative (GPEI)—a consortium made up of Rotary International, the World Health Organization (WHO), UNICEF, the CDC, and more—and other health organizations conducting mass international vaccinations campaigns. But it comes with a disadvantage, too. On rare occasions, the live virus in the OPV can revert to virulence, either causing polio in the person who received the drops, or shedding in their feces and spreading through the environment. Vanishingly small traces of feces on hands or surfaces—even after handwashing—can be sufficient to transmit the virus on the rare instances when this shedding occurs. So far in 2022, there have been 555 cases of polio in 21 countries caused by so-called circulating vaccine-derived poliovirus (cVDPV), according to GPEI. For this reason, the U.S. phased out the use of the OPV in 2000. But much of the rest of the world still uses it.
“In countries where they continue to use OPV,” says Dr. William Schaffner, professor of infectious diseases at Vanderbilt University School of Medicine, “you have more cases of polio that are related to the vaccine than to the wild virus.”
Read More: Routine Childhood Vaccination Rates Fell as Misinformation About the COVID-19 Shot Rose
None of this means that OPV is more menace than boon. The reversion to virulence is rare—happening in about one in three million doses administered, according to Schaffner—and not every case of reversion leads to a case of polio. Since the GPEI began its work in 1988, the OPV is estimated to have prevented 16 million cases of paralysis and 1.5 million deaths. Still, the virus that infected the Rockland County man and turned up in the wastewater in New York is just this type of vaccine-derived virus, presumably carried into the country by someone from a part of the world that uses the OPV. The London and Jerusalem strains are also genetically linked to the New York strain, suggesting an OPV origin.
But the IPV has a drawback, too, in addition to the comparative difficulty and expense of administration. The OPV, since it is taken orally, confers what’s known as gut immunity—meaning that assuming a person who receives the vaccine is not among the unfortunate few in whom the virus reverts to virulence, there is no viral replication in the intestinal system and thus no shedding in feces, even if that person picked up a cVDPV from someone else. The IPV does not establish gut immunity; the vaccine may forever prevent a person who receives the shot from contracting polio, but it doesn’t prevent intestinal replication if that person picks up a cVDPV. That presents a danger, because the IPV-vaccinated person could then spread the cVDPV further.
What’s long been needed is a new oral vaccine: one that establishes gut immunity but is much less likely to revert to virulence. And such a vaccine now exists.
The new oral polio vaccine
In 2021, researchers working with the Bill and Melinda Gates Foundation; the National Institute for Biological Standard and Control (NIBSC) in the U.K.; the University of California, San Francisco; and the U.S. Food and Drug Administration (FDA) developed a novel oral polio vaccine known as nOPV2. (The “2” in the name signifies that it is targeted specifically at polio’s type 2 strain—the only remaining one of the three strains that once existed. Types 1 and 3 have been eradicated.) The nOPV2 vaccine—which isn’t yet approved for use in the U.S.—includes an attenuated virus genetically engineered to be much stabler than the one used in the existing OPV. Rather than having to undergo just a single mutation to revert to virulence, the virus in the nOPV2 must mutate at up to five different points on its genome before it can present a danger.
Read More: RSV Cases Are Rising in Kids and Babies. What Parents Should Know
“It’s a virus that can still accumulate mutations like any virus,” says Raul-Andino Pavlovsky, a professor of microbiology and immunology at the University of California, San Francisco, who was involved in the vaccine development. “But it’s a little bit crippled so it doesn’t evolve as quickly as the original oral polio vaccine, and therefore it’s safer.”
Much safer, actually. “We incorporated changes to make it more faithful as it copied,” says Andrew Macadam, principal scientist with the NIBSC, who also worked on the new vaccine. “With our virus, we’ve never seen reversion to virulence in in vitro tests, in animals or in people.” In March 2021, the new vaccine was first put to work in Africa, and since then, 500 million doses have been administered, especially in Africa, Afghanistan, and Pakistan. In that time, says Macadam, “there’s not been a single verified case of vaccine-associated polio [with the nOPV2].”
How to protect yourself from polio
At the moment, the IPV remains the best means to protect yourself and your family. Currently, 92.5% of U.S. children have received the prescribed 3 doses of the shots by age two, according to the CDC. But vaccination rates vary greatly across the country. In Idaho, the figure is 86.6%, for example, and in the District of Columbia, it’s only 80.4%. In the zip code in which the Rockland County man who recently contracted polio lives, the vaccination rate stands at a dangerously low 37.3%. For that reason, the CDC is considering authorizing the use of the new vaccine in the U.S., hoping to stem the current spread of vaccine-derived poliovirus by establishing gut immunity in people who receive the nOPV2 drops. The new vaccine may be superior to the IPV because of that additional layer of immunity it provides, but more than 20 years of vaccine policy are not overturned quickly—especially since the IPV has been so successful in the U.S.—and the U.S. government is taking its time in deciding whether or not to make the move.
“Out of an abundance of caution, CDC is looking at all options to stop the circulation of poliovirus in New York,” said Jannell Routh, the CDC’s team leader for domestic polio surveillance, in a statement to TIME. On Oct. 19, Routh said, the CDC and New York state formed a polio working group and “began preliminary discussions to consider the criteria under which nOPV2 might be used in areas with persistent circulation of poliovirus.” Any use of the nOPV2 would require emergency use authorization from the FDA, Routh added.
Neither Routh nor other CDC spokespersons would speculate as to when the polio working group would reach a conclusion on whether or not to recommend the use of the nOPV2. For now, Routh said, “vaccinating those at-risk in the affected and surrounding communities with IPV, a safe and highly effective vaccine, continues to remain the priority. Three doses of IPV provides 99% protection against paralytic disease caused by poliovirus infection.”
The nOPV2 is new, and the outbreak in New York is newer still. But at the moment, at least, it’s an old preventive that represents the front line in protecting the vulnerable.
More Must-Reads From TIME
- The 100 Most Influential People of 2024
- Coco Gauff Is Playing for Herself Now
- Scenes From Pro-Palestinian Encampments Across U.S. Universities
- 6 Compliments That Land Every Time
- If You're Dating Right Now , You're Brave: Column
- The AI That Could Heal a Divided Internet
- Fallout Is a Brilliant Model for the Future of Video Game Adaptations
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Write to Jeffrey Kluger at jeffrey.kluger@time.com