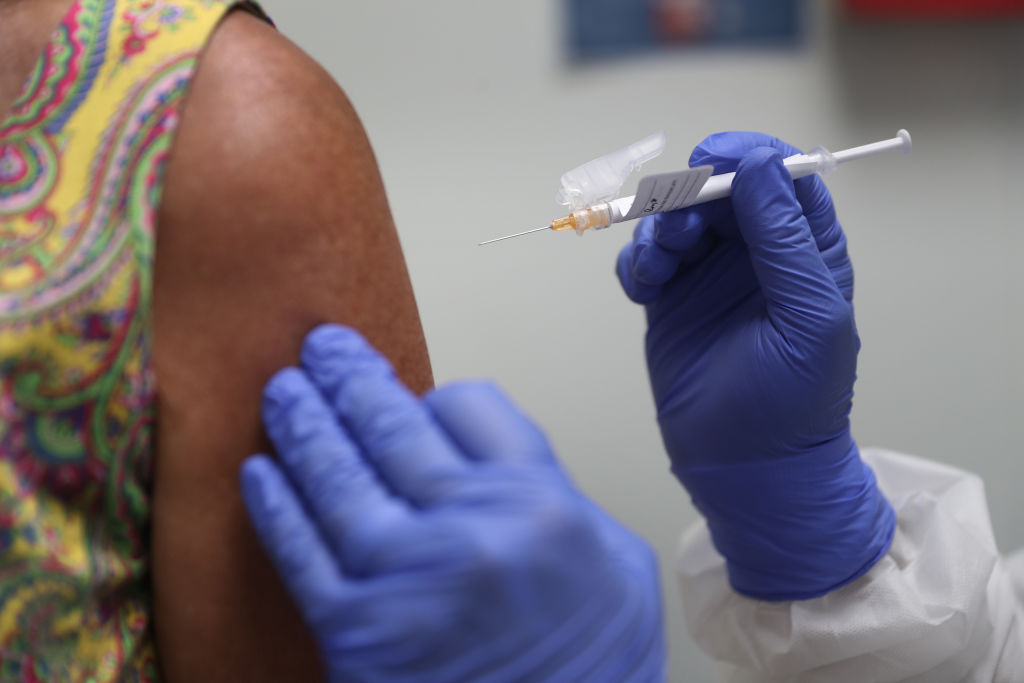
With three vaccine makers saying that their COVID-19 vaccines are at least 90% effective, the U.S. government is gearing up plans to distribute the shots across the country.
In a Nov. 24 briefing, members of the Department of Health and Human Services (HHS)—which oversees the Centers for Disease Control and Prevention (CDC) and the Food and Drug Administration (FDA)—and Operation Warp Speed provided the latest information on the vaccine rollout. Most importantly, HHS Secretary Alex Azar said he’s ready to work with the incoming Biden administration’s transition team on vaccine rollout plans, following a decision by the General Services Administration to begin the handoff process.
“I reiterated my firm commitment that the transition planning and execution will be professional, cooperative and collaborative in the best spirit of looking out for the health and wellbeing of the American people,” Azar said during the briefing. He previously said that he would not initiate transition communications until the GSA decision.
Here’s what the Operation Warp Speed team, which is tasked with supporting development, manufacturing and distribution of COVID-19 vaccines, revealed during the briefing:
An FDA committee will meet Dec. 10 to review Pfizer’s vaccine
A panel of independent experts convened by the FDA will review studies from each vaccine to determine if they are safe and effective enough to distribute to the public. First up are Pfizer and German biotech firm BioNTech, which filed an emergency use authorization (EUA) request for their COVID-19 vaccine on Nov. 20. The FDA group will meet to evaluate the shot, which the companies say is 95% effective in protecting against COVID-19, on Dec. 10.
Moderna is expected to submit a similar request to the FDA soon, and the committee will meet again to evaluate the Massachusetts-based company’s application. AstraZeneca will likely follow as well.
The first batch will include 6.4 million doses
Gen. Gus Perna, chief operating officer of Operation Warp Speed, said that he told state health departments on Nov. 20 that 6.4 million doses of vaccine will be available once the FDA issues the first EUA (at this point, Pfizer’s shots will most likely be the first to get the green light). “What will happen if more becomes available after the initial push is, we will go out following a weekly cadence to distribute [doses] accordingly, with 40 million [doses] by the end of the year.”
How much vaccine each state initially receives will be based on a rough per capita calculation.
Pfizer has conducted dry run shipping drills
Pfizer’s and BioNTech’s vaccine, which is based on a new mRNA technology, needs to be kept at -70 C° to -80 C°. In the U.S., Pfizer has designed special thermal packaging to ship its doses. If replenished with dry ice, the doses can remain in those containers for 15 to 20 days. Once removed, the vials can be stored in a refrigerator for up to five days.
In order to train workers who are receiving the doses, Pfizer has conducted dry runs of shipping its vaccine to 10 locations. Perna said such trials would be done with all 64 public health jurisdictions receiving vaccines from the CDC—most of which are state health departments—to make sure those administering the vaccine are comfortable handling it.
“I’ve personally gone through the process, put my hand in the box, pulled out trays, and timed myself in the execution, and it’s a very, very doable process,” he said. The Pfizer containers will include 975 doses. “We feel confident that if states plan dosages in the right locations, with the drumbeat and cadence of [regular manufacturing], administration of the vaccine to a minimum amount of 975 doses is very doable within 20 days,” he added.
Once the first batch of vaccines are shipped, the next batch will be dispatched within 21 days for the Pfizer vaccine and 28 days for the Moderna vaccine, so people who received their first dose will be able to get their second shot. Once the manufacturing reaches a regular cadence, shipments will be distributed weekly. States will be able to order vaccines through a 24/7 system, and the doses will be shipped the following day.
It will take months until most of the American population can be vaccinated
Vaccine manufacturing will gradually increase as more shots are authorized by the FDA, and people will be vaccinated according to guidelines set by the CDC’s Advisory Committee on Immunization Practices (ACIP), among others. The ACIP recently released principles that it says should guide who gets vaccinated first; these factors include risk as well as equity. Health care workers, first responders and others with essential jobs will be first in line, with the elderly and those with chronic health conditions next. It likely won’t be until next spring or summer that the majority of the American public will be eligible to get vaccinated.
“We are bridging to when we have vaccines first for the most vulnerable like health care workers, first responders and eventually the broad American population,” Azar said. “[Until then] wash your hands, watch your distance and wear face coverings when you can’t watch your distance, and stay out of settings where you can’t do those things.”
More Must-Reads From TIME
- The 100 Most Influential People of 2024
- The Revolution of Yulia Navalnaya
- 6 Compliments That Land Every Time
- What's the Deal With the Bitcoin Halving?
- If You're Dating Right Now , You're Brave: Column
- The AI That Could Heal a Divided Internet
- Fallout Is a Brilliant Model for the Future of Video Game Adaptations
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Contact us at letters@time.com