There’s a step-wise way that cancer doctors go about removing tumors. Generally they start with surgery to cut out as much of the mass as they can, and then follow up with radiation and chemotherapy to zap away any remaining cells the surgeon may have left behind. But finding those cells, some of which are embedded in healthy tissue, is a challenge.
That’s why researchers at Duke University Medical Center, Massachusetts General Hospital and Massachusetts Institute of Technology have developed a probe that can find, stick to and then light up those residual cancer cells, making them easier for surgeons to see. Not only could the technique make cancer surgery more effective, but it could also help doctors to target radiation therapy to just the right parts of a tumor to kill remaining cancer cells.
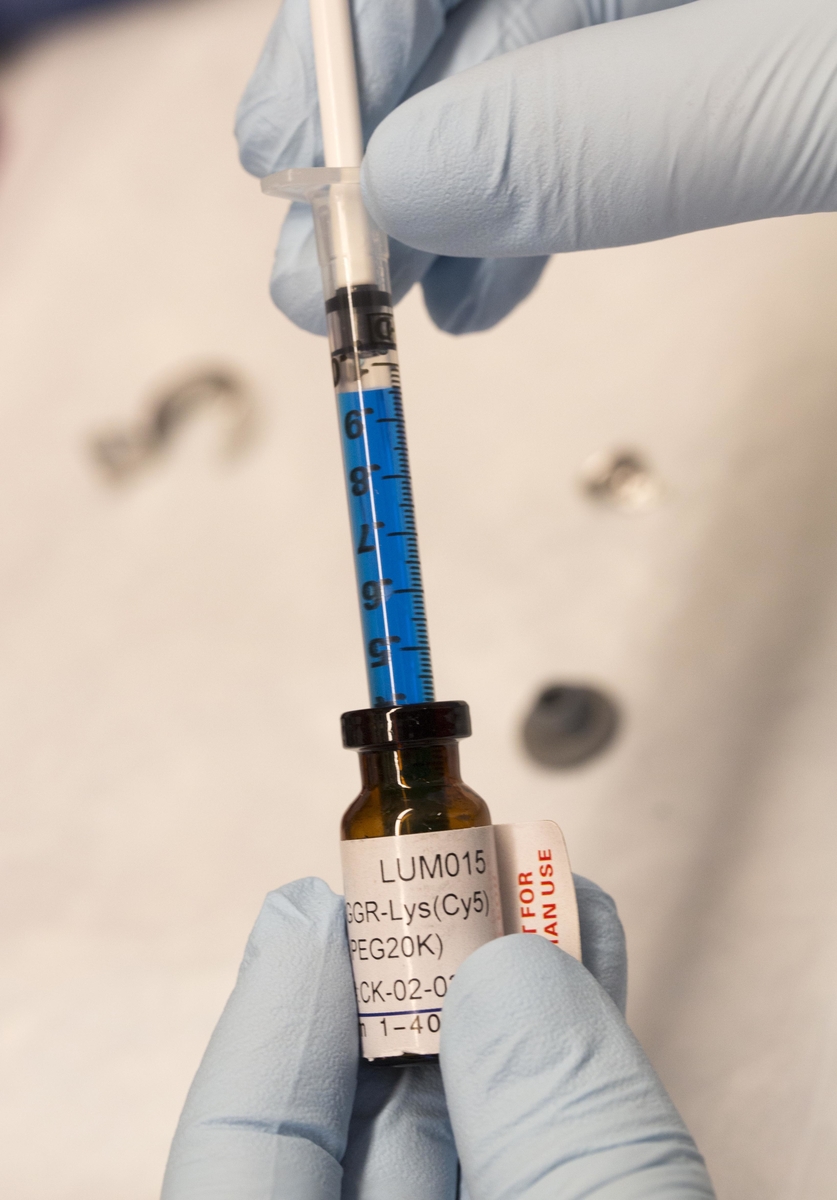
In a study published in Science Translational Medicine, the scientists describe a probe called LUM015 that they injected into areas where surgeons had removed tumors from both mice and people and found that the technique was both safe and potentially effective in detecting cancer.
The mice had soft tissue sarcoma, a cancer that can affect fat, muscles, nerves and lymph vessels as well as the blood. Once LUM015, which is designed to seek out certain markers on cancer cells, finds its target, the probe breaks down and releases a fluorescent agent, making the cancer cells in the animals up to five times brighter, on average, than surrounding healthy tissue like muscle. This gives the scientists a quick way of picking out the cancer cells.
MORE: Painting Tumors: The Technique That Coats Cancer For Easy Identification
The researchers also tested LUM015, which is being developed by Lumicell, in 15 patients with the same cancer or with breast cancer. They found that it was safe and also illuminated tumor cells so they stood out against normal tissue. “The imaging agent preferentially accumulates in tumors,” says Dr. David Kirsch, professor of radiation oncology at Duke University School of Medicine.
One thing that the team needs to work on improving is the efficiency with which LUM015 binds to cancer cells; in the mice, they labeled about 20% of the time. There’s also the issue of whether the probe is binding just to cells that are easily accessible or whether it can find its way deeper into tissues where cancer cells might be hiding. The team is currently doing more detailed studies in patients who have received LUM015 before having their tumors removed.
If those studies continue to support the safety and benefits of LUM015, then the technique may be able to do more than just find residual cancer; it may be used in some way to detect and diagnose cancer in the first place. More work needs to be done to figure out how the fluorescent agent can be given to the entire body, but using it to find leftover cancer is an important first step for this idea.
More Must-Reads From TIME
- The 100 Most Influential People of 2024
- The Revolution of Yulia Navalnaya
- 6 Compliments That Land Every Time
- What's the Deal With the Bitcoin Halving?
- If You're Dating Right Now , You're Brave: Column
- The AI That Could Heal a Divided Internet
- Fallout Is a Brilliant Model for the Future of Video Game Adaptations
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Contact us at letters@time.com