Few issues are more personal—or divisive—than ending a life with a doctor’s lethal prescription.
The issue has sparked national debate recently, after Brittany Maynard, a 29-year-old woman who had terminal brain cancer, went public with her decision to end her own life. She did so on Saturday in Oregon.
Maynard is one of more than 750 people in Oregon who have ingested a lethal dose of prescription medication since the Death with Dignity Act went into effect in 1997. While Oregon has had increased participation over the last 16 years and has spurred similar legislation in other states, aid-in-dying laws remain a lightning rod of contention and deliberation.
Advocates say competent patients should have a right to choose how they die if they are already in the process of dying from a terminal illness. Opponents counter that such a precedent is ripe for abuse.
The battle has been shaped over many years. In the 1990s, Jack Kevorkian assisted in the deaths of more than a hundred terminally ill people to much public outcry. In 2009, politicians sparred over a provision in the Affordable Care Act concerning end-of-life consultations – called “death panels” by critics – to help control health-care costs. (Roughly 28%, or $170 billion, of Medicare is spent on patients’ last six months of life, according to Medicare Newsgroup.)
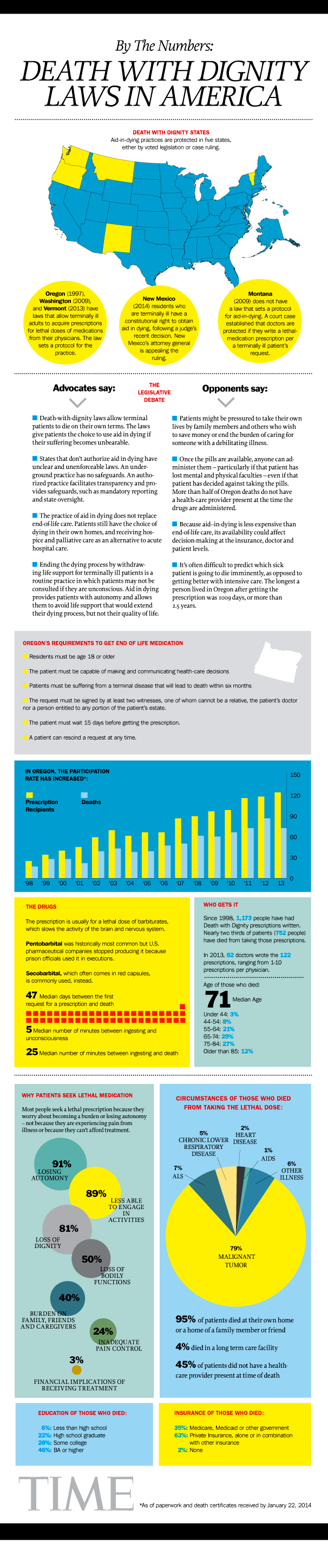
Here is how aid-in-dying laws look today, and a snapshot of the ways in which they are implemented:
More Must-Reads From TIME
- The 100 Most Influential People of 2024
- The Revolution of Yulia Navalnaya
- 6 Compliments That Land Every Time
- What's the Deal With the Bitcoin Halving?
- If You're Dating Right Now , You're Brave: Column
- The AI That Could Heal a Divided Internet
- Fallout Is a Brilliant Model for the Future of Video Game Adaptations
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Contact us at letters@time.com