
This post is in partnership with the History News Network, the website that puts the news into historical perspective. The article below was originally published at HNN.
It began in Nzara, a town inhabited by 20,000 people living in thatch-roofed houses within the dense woods in southern Sudan. Roughly five percent of the population worked in a large cotton factory that was owned by an even larger agricultural company. The factory kept detailed records of its employees’ work hours, perhaps to keep close tabs on absenteeism. Fortunately, it also helped investigators track the pattern of a deadly virus transmission.
On June 27, 1976, one employee would not make it to his work as a storekeeper in the factory. The person, later designated by the initials YG, became very ill, experiencing severe fever, headaches, and chest pains. His brother initially nursed him at home, located 10 kilometers from the factory in a remote and rural area south of Nzara. Three days later, with his condition worsening, he was brought to the Nzara hospital – a small and ill-equipped facility that typically did not admit a lot of patients. By the fifth day he was bleeding from the mouth and nose. He began to suffer from bloody diarrhea. Nine days after his illness began, YG died. His brother became ill a week later but survived.
One of YG’s co-workers, BZ, who was also a storekeeper, was admitted to the same hospital on July 12, six days after YG died. This second storekeeper died on July 14. On July 19, the second storekeeper’s wife also died from the same illness. A third factory employee, PG, worked in the cloth room next to the store.
In contrast to YG and BZ, who usually stayed close to home and had few friends, PG was an outgoing bachelor who lived at the center of town and was quite well known in the area. PG and his two brothers, Samir and Sallah, lived with a merchant, MA. The brothers were active in their community and organized social events such as dances. When PG fell ill in late July, many of his friends naturally came to visit. Two women in particular, HW and CB, were kind enough to nurse him during the first days of his illness. His condition apparently deteriorated rapidly as he succumbed to infection three days later. Samir became ill a day before PG died, and together with Sallah, they travelled 128 kilometers east to Maridi where Samir was admitted to the Maridi hospital. Sallah assisted in caring for his brother who died on August 17. A day later, Samir himself became sick and died not too long after. By this time, the two women who cared for PG, as well as another factory worker and a nurse in Nzara hospital had died from the same disease. Investigators later determined that 48 cases and 27 deaths could be traced to exposure to PG – the ebullient, outgoing bachelor of Nzara.
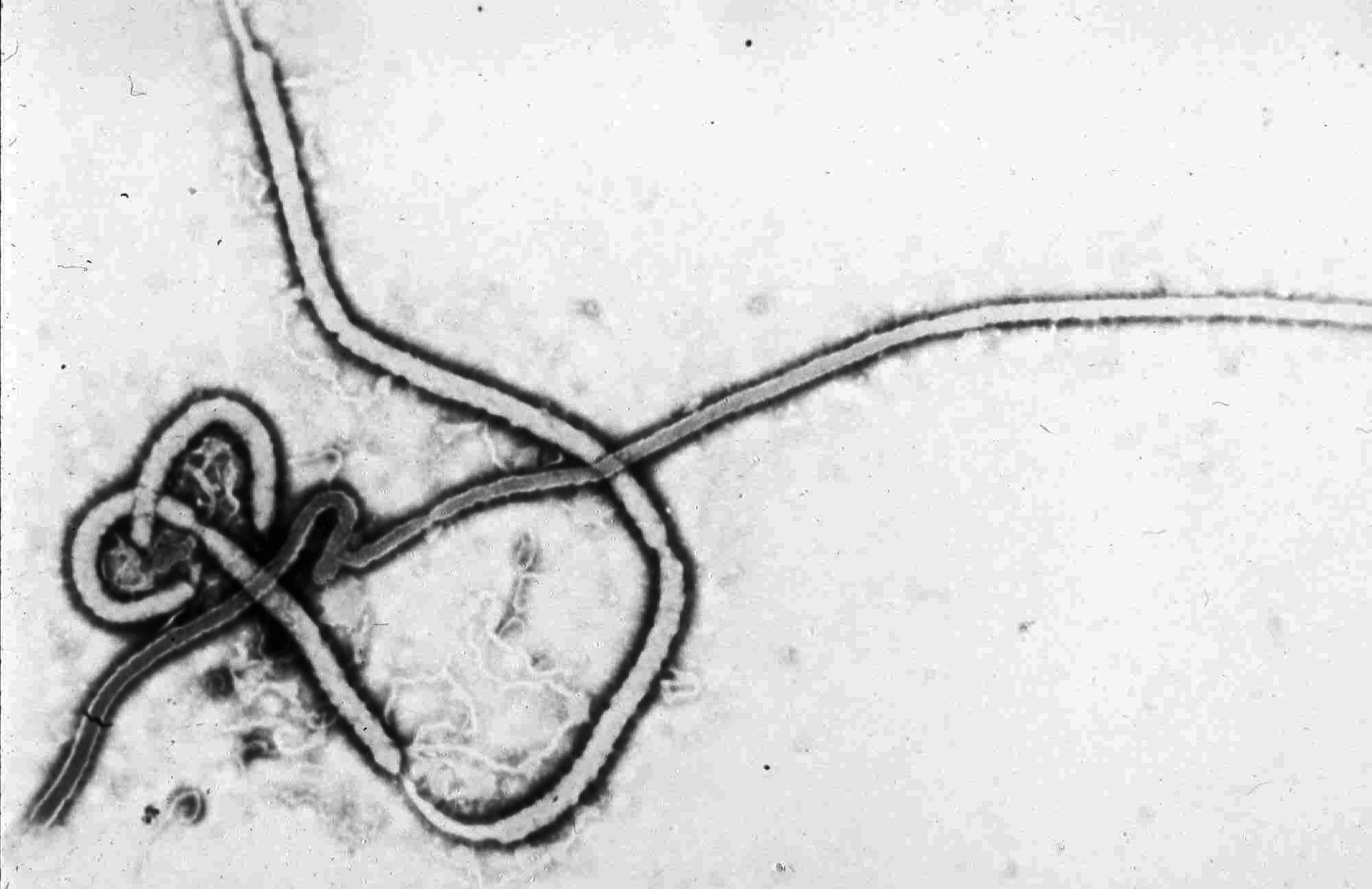
During this first Ebola outbreak in southern Sudan that started in June 1976, 248 cases were identified. Fifty-three percent of the victims died. Investigators identified the cotton factory in Nzara as the source of the infection. Most of the victims, however, were actually infected in Maridi, which ironically had a more active and larger hospital where transmission of the virus was amplified. By the end of the year, the epidemic also hit the Democratic Republic of Congo (DRC), infecting more than 300 people and killing almost 90% of the victims.
In late October of 2014, the World Health Organization reported nearly 10,000 Ebola Virus Disease cases from the 2014 outbreak. Nearly all the cases were in Liberia, Sierra Leone, and Guinea. The fatality rate was nearly 50%. Thirty-five years after the initial Ebola outbreak, it is chilling to see the similar pattern of risk of transmission, particularly to the individuals who care for the Ebola victims, being mirrored even within 21st century hospitals.
Rod Tanchanco is a physician specializing in Internal Medicine. He writes about events and people in the history of Medicine. His personal blog is at talesinmedicine.com.
More Must-Reads From TIME
- The 100 Most Influential People of 2024
- Coco Gauff Is Playing for Herself Now
- Scenes From Pro-Palestinian Encampments Across U.S. Universities
- 6 Compliments That Land Every Time
- If You're Dating Right Now , You're Brave: Column
- The AI That Could Heal a Divided Internet
- Fallout Is a Brilliant Model for the Future of Video Game Adaptations
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Contact us at letters@time.com