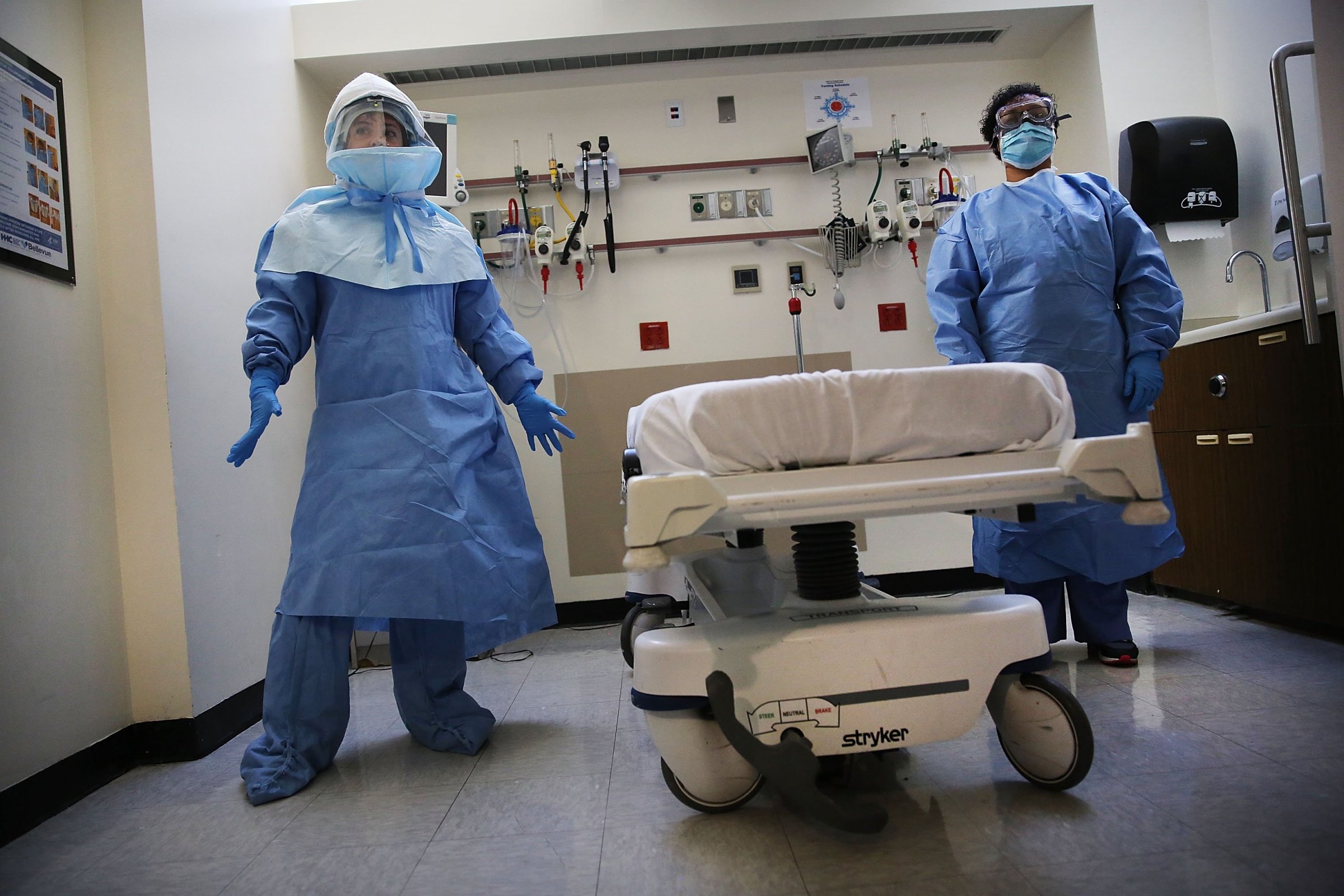
A health care worker who had “extensive” contact with Dallas Ebola patient Thomas Eric Duncan has been infected with Ebola.
“We don’t know what occurred, but at some point there was a breach in protocol,” Centers for Disease Control and Prevention (CDC) director Dr. Tom Frieden said in a meeting with the press Sunday. The Dallas hospital worker is the second health care worker in the Western world to be infected with the disease, which begs the question: Are all hospitals really capable of caring for a patient with Ebola, as Americans have been repeatedly told?
The CDC is still insisting yes, but hospitals need to start listening very carefully to their guidance. The CDC has long been advising hospitals on how to take care of a potential patient, but the agency is kicking it up a notch this week given the new patient and Texas Health Presbyterian Hospital’s blunders, including not admitting Duncan the first time he arrived at the hospital with a 103-degree fever.
The CDC is sending in a team of six to eight disease specialists to Dallas to help with infection control, a CDC spokesperson told TIME. A couple of those members just returned from Dallas on Friday, but given the new infection, they’re hopping back on the plane to help the hospital. “As that team continues to investigate what happened [at Texas Health Presbyterian Hospital], it will be used as a lesson learned experience,” says CDC. President Obama also directed the CDC on Oct. 12 to investigate.
Every hospital in the U.S. has the equipment and isolation areas needed to treat someone with Ebola, but there’s no denying that the physicians at Emory University hospital, for example, have more experience and training. TIME visited the infectious disease team at Emory in August, and the team had been training for a situation like Ebola for 12 years, undergoing drills at least twice a year. That’s not the case at most medical facilities.
“You’re going to see us really making even more clear what hospitals need to be doing,” says the CDC spokesperson. “We are really trying to help health care workers understand the principles [they] need to follow and why, and how to do them.” The CDC received a 10-fold increase in calls from hospitals after a nurse in Spain was infected with Ebola.
1. Have a lead manager. Frieden said the CDC is recommending that hospitals have someone’s whose role it is to monitor the protocols that physicians and nurses are taking for protection. Taking on and off the protective equipment is one of the most high-risk scenarios and has to be done meticulously. “[Treating Ebola] can be done safely, but it’s hard to do safely,” Dr. Frieden said in the press conference, adding that even a single slip can result in contamination.
2. Learn from the country’s best. On Oct. 14, doctors at Emory and Nebraska—both best-in-class facilities when it comes to treating something like Ebola—will host a conference call for health care workers. On Oct. 21, the CDC and the Partnership for Quality Care will be hosting a live educational meeting in New York to show health care workers how to prepare their facilities and themselves. The CDC says the goal is to get 5,000 front-line health care workers there in person, and to also live stream it for those who cannot attend in person. The CDC has long been running a Health Alert Network that hospitals and individuals can subscribe to for notifications and advice on caring for diseases.
3. Get a patient’s travel history. The CDC says health workers should consider the possibility of Ebola if a patient exhibits fever, severe headache, abdominal pain, vomiting, diarrhea, or unexplained bleeding or bruising. If a patient has been to Ebola-affect countries, “immediate action should be taken.”
4. Isolate immediately. If a patient might have Ebola, they should be “isolated in a single room (with a private bathroom), and healthcare personnel should follow standard, contact, and droplet precautions, including the use of appropriate personal protective equipment (PPE).”
5. Be protected. PPE should consist of gloves, gown, eye protection (goggles or face shield), and a face mask. In situations where there may be copious amounts of bodily fluids like blood, vomit and feces, health workers should consider double gloving, wearing disposable shoe covers and leg coverings. Some hospitals may choose hazmat suits, since those suits are made up of fewer pieces—which means it’s less for doctors to take on and off.
You can read more of the CDC’s recommendations here.
More Must-Reads From TIME
- The 100 Most Influential People of 2024
- The Revolution of Yulia Navalnaya
- 6 Compliments That Land Every Time
- What's the Deal With the Bitcoin Halving?
- If You're Dating Right Now , You're Brave: Column
- The AI That Could Heal a Divided Internet
- Fallout Is a Brilliant Model for the Future of Video Game Adaptations
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Contact us at letters@time.com