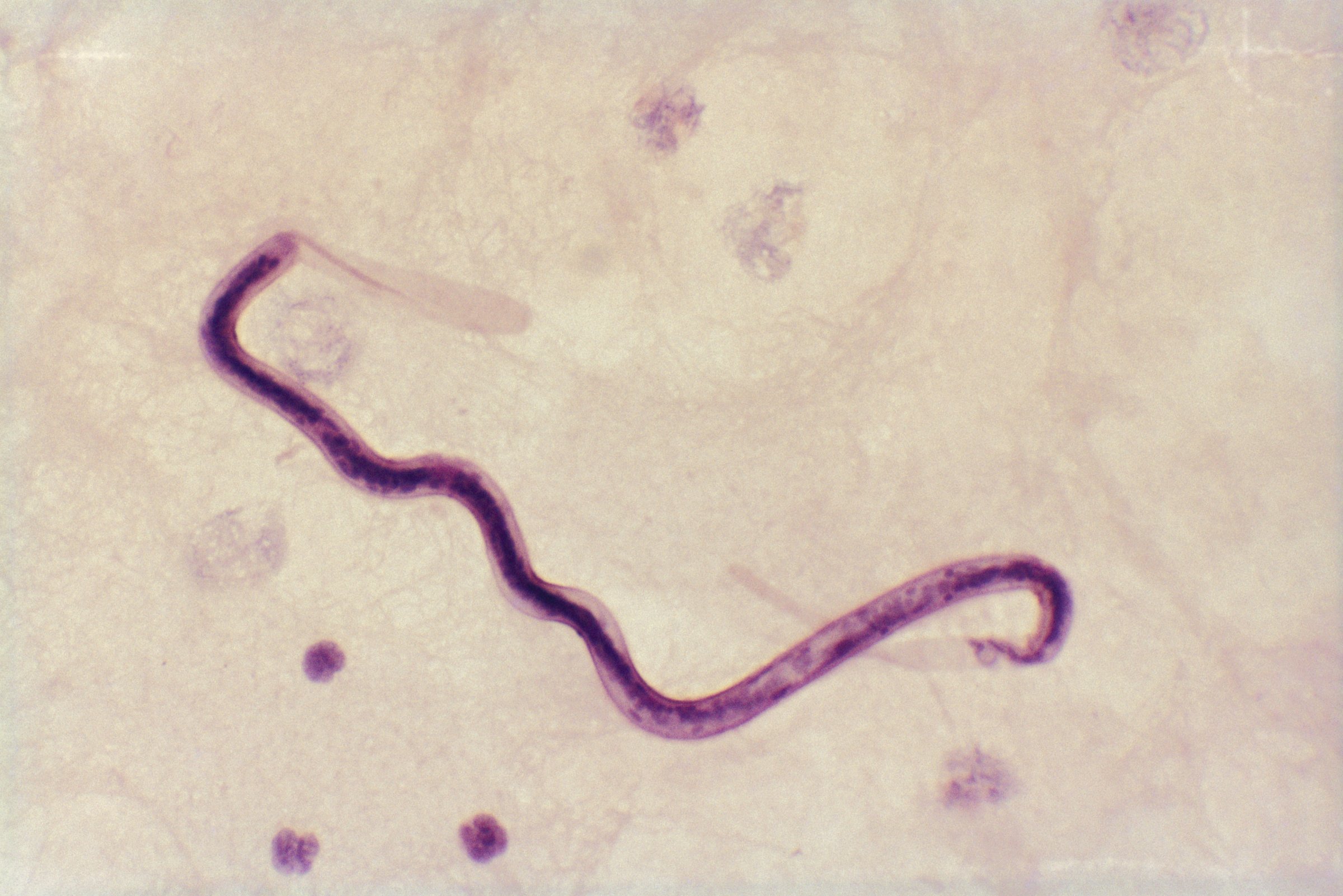
Parasitic worms plaguing Africa may soon meet their match—because now, there’s an app for them, too. According to a new report in the journal Science Translational Medicine, researchers have developed a way to rapidly test for a particularly troublesome kind of eye worm through an iPhone.
Worms are a huge problem in parts of Central and West Africa. A single species called O. volvulus causes “river blindness,” the second-biggest cause of infectious blindness in the world, and another, W. bancroftiis, causes lymphatic filariasis, the second leading cause of disability in the world.
The good news is that they can be cured with an anti-parasitic drug called ivermectin. The bad news is that a third kind of worm—a particularly disgusting kind called Loa loa, or African eye worm—makes treatment much more risky. Loa loa wriggle out of the eye when they mature and spread throughout the body, but even though they look terrifying, they’re not life-threatening. However, when people harbor high quantities of these worms and take the antiparastic drug ivermectin, they can suffer fatal brain damage within days. That enormous side effect has stopped mass drug administration in its tracks, putting the effective drug on ice and countless at risk for blindness and disability.
Finding people with high levels of this worm is extremely important, but screening takes days and requires resources. In order to test levels, technicians have to make a blood smear on a glass slide, stain the sample to highlight the worms and manually count them under a microscope. But now, engineers at the University of California, Berkeley, have developed a method that takes just three minutes using a smartphone device called CellScope Loa.
Here’s how it works: you slide your iPhone into a small 3D-printed box, which is built with microprocesssors, a motor and some LEDs for illumination. Align the phone camera with lenses in the box, and after a quick fingerprick for blood and the push of a button, the phone takes five short videos of worms wriggling in the blood and wirelessly analyzes the sample with the help of an app. The microscope senses the motion of the Loa loa, and within a matter of seconds, a worm count pops up on the screen.
See the Human Body Under a Microscope





The researchers tested the CellScope on 33 people in Cameroon and compared that analysis against the gold-standard smear technique. The diagnoses and very low false-negative rates matched.
Being able to diagnose worms with one streamlined portable device has a lot of advantages over current testing methods, which involve bulky microscope, a computer, a laboratory and a lot of time and money, says Daniel Fletcher, head of the lab that designed CellScope and associate chair and professor of bioengineering at UC Berkeley. Teams that provide mass drug administration services will be able to take the CellScope to villages, filter out who shouldn’t be treated and give worm medication to the rest, he says.
Next, the team will test the device on 40,000 people in Cameroon.
It’s possible that the device will have implications far beyond the African eye worm. “Right now, we’ve designed the algorithms to look for this particular kind of worm,” Fletcher says. “But we’re hopeful that the general strategy of using all parts of the phone—not just the camera, but using its ability through Bluetooth to control other components, its computing ability to analyze images, and the screen to report results—could be applicable to a range of other resources.”
More Must-Reads From TIME
- The 100 Most Influential People of 2024
- The Revolution of Yulia Navalnaya
- 6 Compliments That Land Every Time
- What's the Deal With the Bitcoin Halving?
- If You're Dating Right Now , You're Brave: Column
- The AI That Could Heal a Divided Internet
- Fallout Is a Brilliant Model for the Future of Video Game Adaptations
- Want Weekly Recs on What to Watch, Read, and More? Sign Up for Worth Your Time
Write to Mandy Oaklander at mandy.oaklander@time.com